Full Skin Exams
in Beverly Hills, CA
Couture Dermatology specializes in treating melasma in Beverly Hills, CA, offering advanced solutions for this common skin condition. Melasma causes brown or gray-brown patches, typically on the face, and is often triggered by sun exposure or hormonal changes. Our experienced dermatologists provide personalized care to help restore a clear, even complexion.

Understanding Melasma
Common Signs and Symptoms of Melasma
Facial Discoloration
Patchy Pigmentation
Sun-Exposed Area Changes
Symmetrical Patterns
Gradual Onset
Main Causes of Melasma
Top Treatments for Melasma
- Topical creams with hydroquinone help lighten dark patches.
- Chemical peels exfoliate the skin and reduce pigmentation.
- Laser therapy targets deeper pigment for stubborn melasma.
- Microneedling stimulates collagen and can improve skin tone.
- Prescription retinoids promote cell turnover and fading.
- Daily sunscreen use prevents melasma from worsening.
Who Is a Good Candidate
- Individuals with visible brown or gray patches on the face.
- People experiencing pigmentation changes due to sun exposure or hormones.
- Those seeking professional solutions for uneven skin tone.
- Patients who have not responded to over-the-counter products.
Check Your Insurance Coverage
Melasma Treatment Benefits
Restores Even Skin Tone
Boosts Self-Confidence
Customizable Treatment Options
Minimally Invasive Solutions
Dr. Chinonso Kagha
Abisogun, MD, FAAD
Why Choose Couture Dermatology For Your Melasma Treatment?
At Couture Dermatology, our board-certified dermatologists have extensive experience in diagnosing and treating melasma with the latest, evidence-based therapies. We take a personalized approach, tailoring every treatment plan to each patient’s skin type, lifestyle, and unique needs. Our commitment to advanced technology and compassionate care ensures you receive the highest standard of treatment for optimal results in a welcoming environment.
Check Your Insurance Coverage
Testimonials

- Rosie D.
Healthy Skin.
Beautiful
Complexion.
A More Confident You.
Full Body Skin Exams. Annual. Thorough. Dermoscopy.
Skin cancer is the most common cancer in the United States — and the most survivable when caught early. A full body skin examination by a board-certified FAAD dermatologist, performed annually, is the most effective available tool for detecting basal cell carcinoma, squamous cell carcinoma, and melanoma before they progress. At Couture Dermatology, every skin exam is conducted with dermoscopy — a magnification technique that improves diagnostic accuracy for melanoma by approximately 30% over the naked eye — and biopsies are performed in-office on the same visit when clinically indicated.
skin cancer by age 70
with dermoscopy
dermatologist
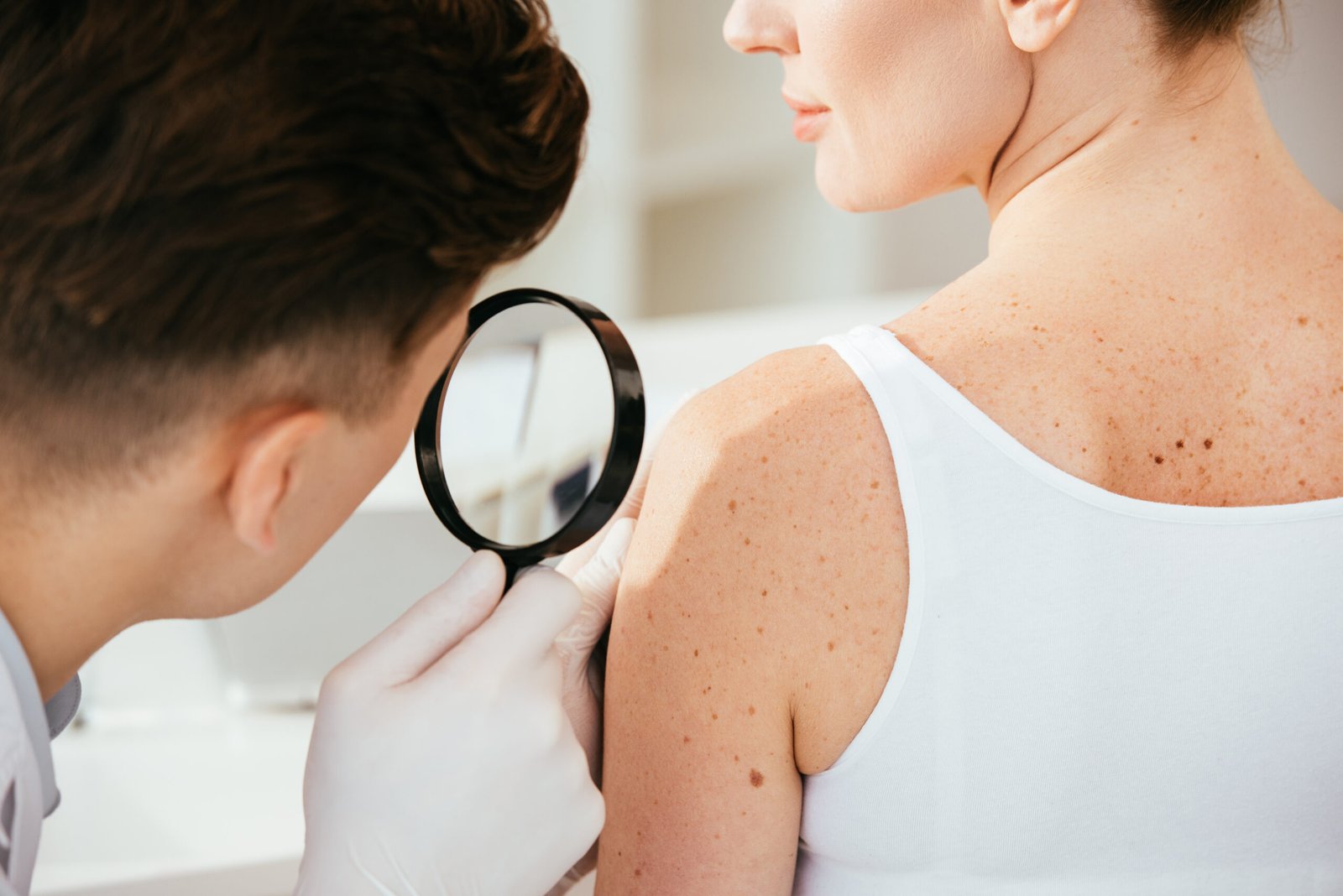
"The best outcome in skin cancer is the one that never requires treatment beyond a simple in-office biopsy — because it was caught early."
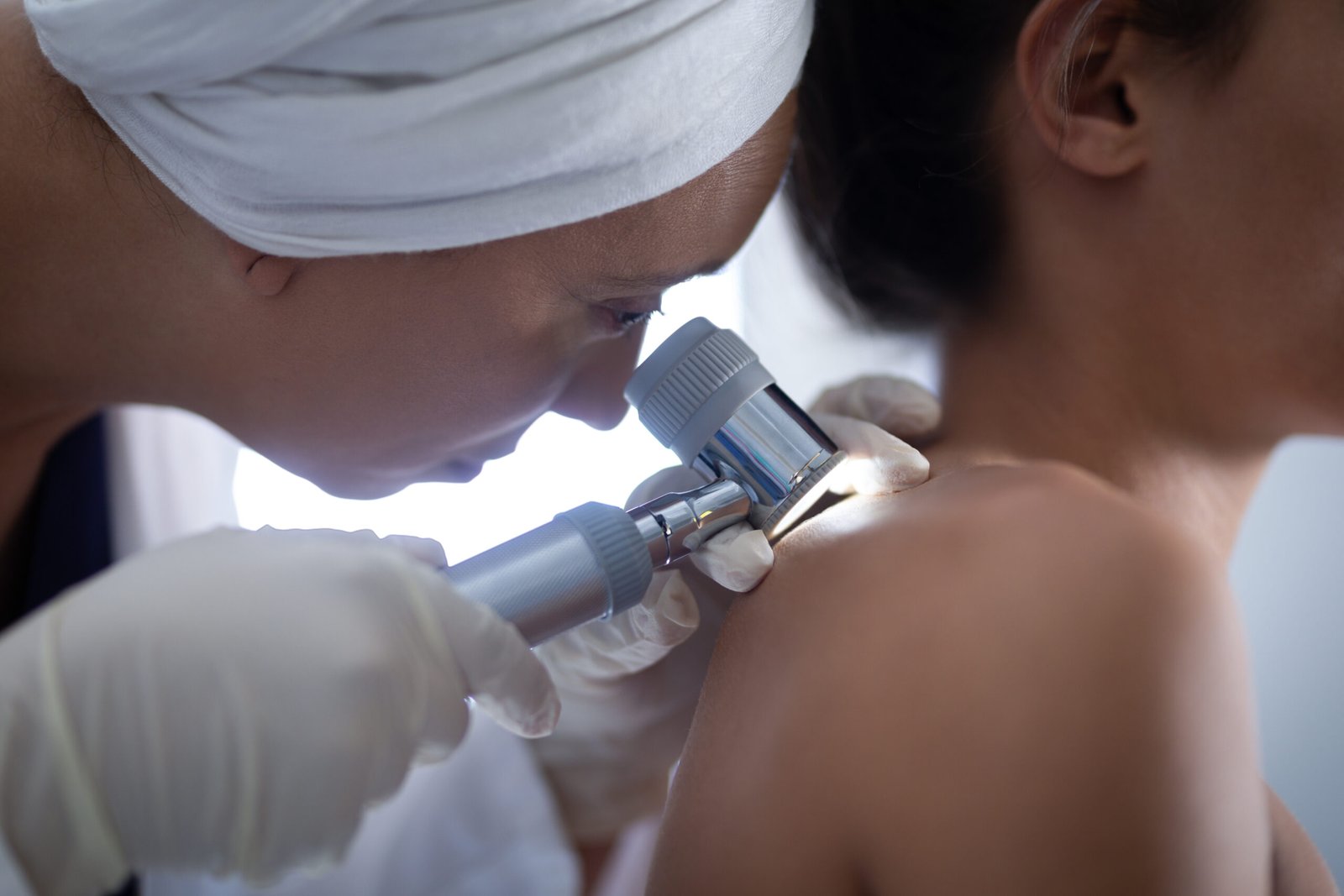
A Systematic Head-to-Toe
Examination of Every Skin Surface.
A total body skin examination (TBSE) is a systematic, methodical examination of every skin surface — scalp, face, ears, neck, chest, abdomen, back, arms, hands, groin, genitals, legs, feet, and soles — conducted by a board-certified dermatologist. It is not a cursory visual sweep; it is a structured clinical assessment in which each anatomical area is examined in sequence using both naked-eye inspection and dermoscopy on any lesion that warrants further evaluation.
Dermoscopy — also called dermatoscopy or epiluminescence microscopy — uses a handheld lens that magnifies the skin surface ×10 to ×40 with polarised light, eliminating surface reflection and revealing the subsurface pigment architecture, vascular patterns, and structural features invisible to the naked eye. The blue-white veil, atypical pigment network, regression structures, irregular streaks, and atypical vascular patterns that characterise early melanoma are identified dermoscopically before they are visible without magnification. In trained hands, dermoscopy improves melanoma diagnostic sensitivity by approximately 30% over the unaided eye and reduces unnecessary biopsies of benign lesions.
The exam concludes with a clear communication of every finding — what was seen, what was evaluated dermoscopically, what was considered benign, and what requires either monitoring, biopsy, or further assessment. Where a biopsy is indicated, it is performed at the same appointment. Patients leave with a clear understanding of every decision made during the exam.
The Three Primary Skin Cancers
and What They Look Like.
Skin cancer is not a single disease. Basal cell carcinoma, squamous cell carcinoma, and melanoma have distinct appearances, locations, and risk profiles — and different urgency for treatment. Recognising each is the purpose of the annual skin exam.
Basal Cell Carcinoma
Basal cell carcinoma (BCC) is the most common human cancer — accounting for approximately 80% of all skin cancers — arising from basal cells in the deepest layer of the epidermis. It grows slowly, almost never metastasises, but causes progressive and potentially significant local tissue destruction if left untreated. BCC is almost exclusively found on chronically sun-exposed skin: the face (nose, cheeks, periorbital area), scalp, neck, ears, and upper chest. The classic presentation is a pearly or translucent papule with telangiectatic vessels at the surface and a central depression or ulceration — the "rodent ulcer" — though BCC appears in multiple morphological subtypes. Superficial BCC appears as a flat pink-red scaly patch, most commonly on the trunk. Morphoeic (sclerosing) BCC presents as an ill-defined, scar-like, firm area and is the most infiltrative and difficult-to-clear subtype, requiring wider surgical margins. Dermoscopy of BCC reveals arborising (tree-like) vessels, blue-grey ovoid nests, and spoke-wheel structures specific to this cancer. Treatment is by surgical excision or Mohs micrographic surgery for high-risk locations; superficial BCC can be treated with topical imiquimod or photodynamic therapy in appropriate cases.
Squamous Cell Carcinoma
Squamous cell carcinoma (SCC) arises from keratinocytes — the primary cells of the epidermis — and accounts for approximately 20% of skin cancers. Unlike BCC, SCC has meaningful metastatic potential: overall metastatic risk is approximately 4%, rising substantially in high-risk variants (SCC of the lip, ear, or scalp; SCC arising in scars or chronic wounds; SCC greater than 2cm; SCC in immunosuppressed patients; poorly differentiated SCC). Early-stage SCC appears as a firm, scaly, keratotic plaque or nodule on sun-damaged skin — the lips, ears, dorsum of the hands, scalp, and lower legs. SCC in situ (also called Bowen's disease) is the precancerous form, presenting as a well-defined, persistent, scaly pink-red plaque that has not yet penetrated the basement membrane. Actinic keratosis (AK) — the precursor lesion — appears as a rough, sandpaper-textured patch on sun-exposed skin and progresses to invasive SCC in approximately 0.5–1% of lesions per year. Actinic keratoses are identified, counted, and treated at skin exams — either with cryotherapy, topical 5-fluorouracil, imiquimod, tirbanibulin, or photodynamic therapy depending on the number, distribution, and patient factors.
Melanoma
Melanoma arises from melanocytes — the pigment-producing cells of the epidermis — and is the most dangerous form of skin cancer. Although melanoma accounts for only approximately 1% of skin cancers, it is responsible for the majority of skin cancer deaths. The 5-year survival for in situ melanoma or thin invasive melanoma (Breslow thickness less than 1mm) exceeds 95%; advanced metastatic melanoma (stage IV) carries a substantially worse prognosis, though survival has improved markedly since the introduction of immune checkpoint inhibitors and BRAF-targeted therapy. The most important determinant of outcome is Breslow depth at diagnosis — every additional millimetre of invasion significantly worsens prognosis. This is precisely why annual screening is not optional for high-risk patients: the difference between melanoma detected at 0.3mm and at 4mm is, literally, the difference between a wide local excision and a stage III or IV cancer requiring systemic therapy. Melanoma is identified by the ABCDE rule and confirmed by dermoscopy, with excision biopsy for histological staging. Nodular melanoma — which grows vertically rather than radially — is the variant most commonly missed on self-examination as it does not follow the classic ABCDE pattern.
The ABCDE Rule for
Melanoma Warning Signs
Monthly self-examination between annual professional skin exams is recommended. These are the visual warning signs of melanoma to look for — any lesion meeting one or more criteria warrants evaluation. Note that nodular melanoma and amelanotic melanoma may not follow this pattern.
One half of the lesion does not mirror the other. A benign mole, drawn through the centre, would produce two roughly equal halves. Melanoma typically lacks this symmetry — one half is larger, differently shaped, or differently coloured than the other.
Irregular, ragged, notched, or blurred edges — rather than the smooth, well-defined border of a benign mole. The border of a melanoma often looks as though the pigment is spreading unevenly into the surrounding skin, or has an indistinct, fuzzy edge.
Variation in colour within a single lesion — multiple shades of brown, black, red, white, or blue. A benign mole is typically one uniform shade of brown. Colour variation within a single lesion is one of the most sensitive indicators of melanoma on dermoscopy.
Greater than 6mm at its widest point — approximately the diameter of a pencil eraser. Most benign moles are smaller. Melanomas are often larger at the time of diagnosis, though they can be diagnosed earlier when smaller if the other ABCDE features are present.
Any change in size, shape, colour, or new symptoms — bleeding, itching, crusting, or pain — in a lesion that was previously stable. Evolution is arguably the most important criterion: a mole that was benign last year but has changed this year demands evaluation regardless of whether it meets the other ABCDE criteria.
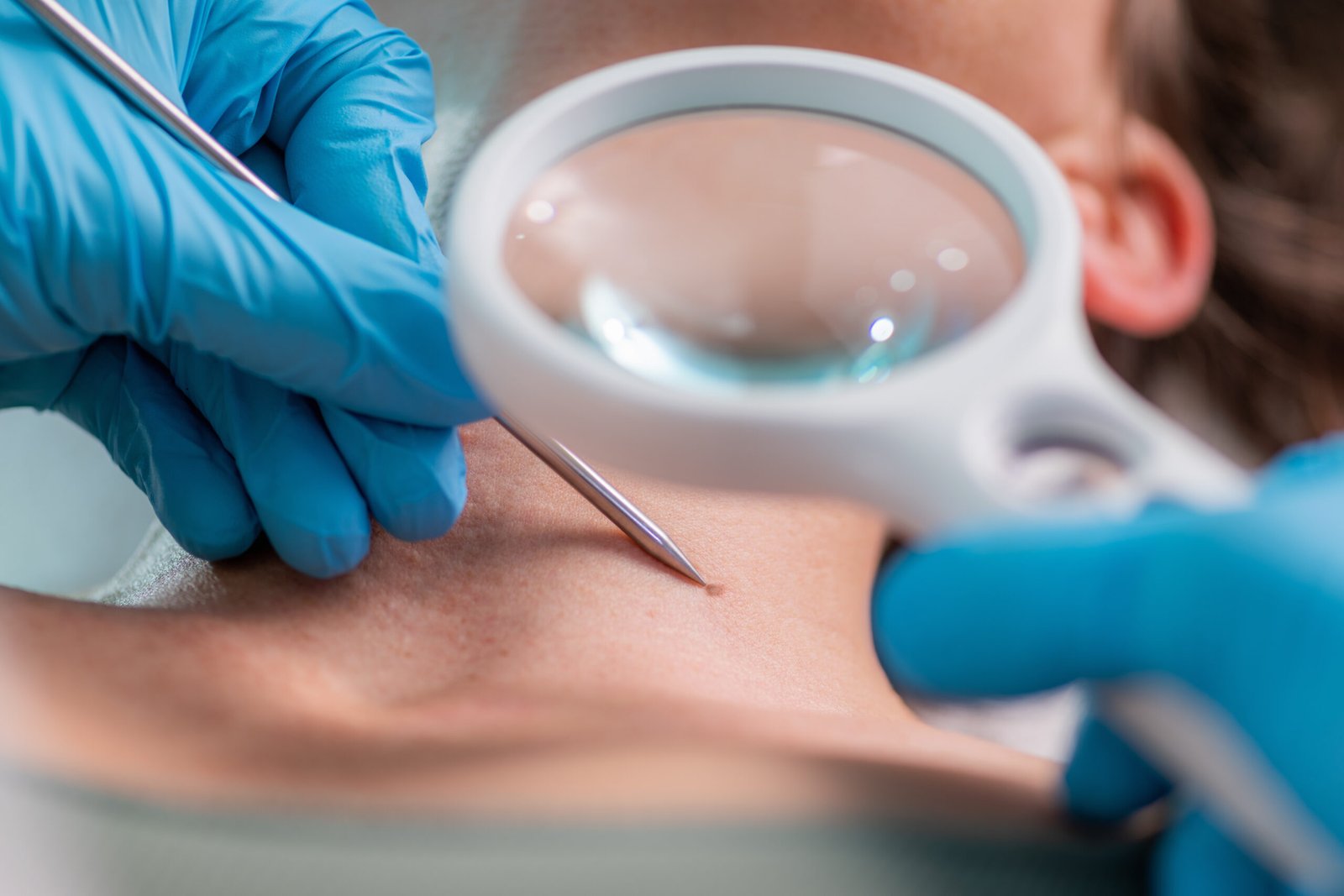
When a Biopsy Is Needed.
Same Day, In-Office.
When a lesion identified during the skin exam warrants tissue diagnosis — because dermoscopy reveals features that cannot be confidently assessed as benign, or because the clinical history is concerning — a biopsy is performed at the same appointment. There is no need to return for a separate procedure visit. The type of biopsy depends on the suspected diagnosis and the lesion morphology.
A shave biopsy removes the superficial layer of a lesion using a curved blade and is appropriate for raised, exophytic, or clinically low-suspicion pigmented lesions. An excisional biopsy removes the entire lesion with a narrow margin and is the preferred approach for a lesion with dermoscopic features suspicious for melanoma — where complete lesion architecture is required for accurate Breslow depth measurement and histological staging. A punch biopsy uses a circular cutting tool of 2–6mm diameter and is appropriate for flat lesions requiring full-thickness dermal sampling, including inflammatory dermatoses and some pigmented lesions. All biopsy specimens are processed by a dermatopathologist.
Results are typically available within 5–7 business days. Your dermatologist contacts you directly to communicate the result and discuss the clinical significance. Where the biopsy confirms a skin cancer, the next step — whether wide local excision, Mohs micrographic surgery referral, or further staging — is explained clearly with the reasoning behind it.
From Booking to
Results
History & Risk Assessment
Your dermatologist begins with a review of your skin cancer risk factors: personal history of skin cancer or actinic keratoses; family history of melanoma; lifetime sun exposure history including occupational exposure, sunbathing history, and tanning bed use; history of severe blistering sunburns, particularly in childhood; immune status including current or prior immunosuppressive medications; and any specific lesions you have noticed or are concerned about. This directs where particular attention is paid during the exam.
5–10 minutesFull Body Examination
You will be asked to undress to underwear and provided a gown. The dermatologist systematically examines every skin surface: scalp (often with a comb to part the hair), face, ears, neck, chest, abdomen, back, arms, hands including between the fingers and under the nails, genital area, legs, feet, and soles including between the toes. Gown positioning is adjusted methodically as each area is examined — no skin surface is excluded. Dermoscopy is applied to all moles and any area that warrants closer evaluation. The exam typically takes 20–30 minutes.
20–30 minutesDermoscopy & Decision
Every mole and pigmented lesion is assessed dermoscopically. Lesions are classified as confidently benign (no further action), requiring monitoring (baseline photograph taken, specific feature to watch for, return interval recommended), or requiring biopsy for tissue diagnosis. The dermoscopic features driving each decision are explained — patients are shown what was seen and why it was assessed as it was. Photography of monitored lesions is performed for baseline documentation.
Explained in fullBiopsy If Indicated
If a biopsy is required, it is performed at the same appointment under local anaesthetic. The area is cleaned and anaesthetised with a small injection — the anaesthetic itself is the most uncomfortable moment; the biopsy is painless once numb. The specimen is submitted to a dermatopathologist. Results are typically available in 5–7 business days. Your dermatologist will call you with the result and discuss the next step, whether that is reassurance, a short follow-up visit, wide excision, or Mohs surgery referral. Biopsy sites are small, heal within 1–3 weeks with simple aftercare, and leave minimal scarring in most locations.
Same-day · Results 5–7 daysRisk Factors That Elevate
Your Skin Cancer Risk
Annual screening is recommended for all adults. These factors indicate elevated risk — and typically justify more frequent monitoring, every 6–12 months, or specialist referral.
Prior Skin Cancer or Atypical Moles
A personal history of any skin cancer — BCC, SCC, or melanoma — is the single strongest predictor of future skin cancer. Up to 50% of patients treated for one BCC will develop another within 5 years. Patients with a prior melanoma require close monitoring — typically every 3–6 months — to detect recurrence and new primary melanomas. Atypical (dysplastic) moles — clinically irregular, histologically dysplastic — are independent risk markers; dysplastic nevus syndrome (multiple atypical moles) is associated with significantly elevated melanoma risk.
Fair Skin, Light Eyes & Red or Blonde Hair
Fitzpatrick skin types I and II — those who burn easily, tan poorly, and have fair or ruddy complexions — have the lowest constitutive melanin protection and the highest UV damage accumulation per unit of sun exposure. Light-coloured eyes (blue, green, grey) and red or blonde hair are phenotypic markers of the same low-melanin genetic profile and are independent risk factors for melanoma. In Southern California's year-round high UV environment, fair-skinned individuals accumulate significant lifetime UV damage even without intentional sunbathing.
Significant Lifetime UV Exposure
Cumulative UV exposure from outdoor work, time in high-altitude or equatorial environments, recreational sun exposure over decades, and — importantly — indoor tanning bed use all elevate skin cancer risk. Tanning bed use before age 35 increases melanoma risk by approximately 75%. Total lifetime UV dose is the primary environmental determinant of BCC and SCC risk; episodic intense UV — particularly blistering sunburns — is the primary environmental contributor to melanoma risk alongside cumulative dose.
Family History of Melanoma
A first-degree relative (parent, sibling, or child) with a history of melanoma approximately doubles an individual's melanoma risk. Familial atypical multiple mole melanoma syndrome (FAMMM) — characterised by multiple atypical moles and melanoma in two or more first-degree relatives — carries a substantially elevated lifetime risk. The CDKN2A and CDK4 genes are associated with familial melanoma susceptibility, and genetic counselling may be appropriate for patients with strong family histories.
Organ Transplant Recipients
Solid organ transplant recipients on long-term immunosuppression — typically tacrolimus, cyclosporin, or azathioprine — have dramatically elevated skin cancer risk. SCC risk is increased approximately 65–250-fold; BCC risk approximately 10-fold. Immunosuppression impairs immune surveillance of UV-mutated keratinocytes, allowing SCCs to develop and progress more rapidly and with higher metastatic potential than in immunocompetent individuals. Transplant recipients should be seen by a dermatologist every 3–6 months, and sun protection is of particular clinical importance in this population.
History of Blistering Sunburns
Severe blistering sunburns — particularly those occurring in childhood and adolescence, when melanocyte DNA damage is most consequential — are strongly associated with melanoma risk independent of cumulative UV exposure. Five or more blistering sunburns between the ages of 15 and 20 are associated with an approximately 80% increase in lifetime melanoma risk. Sunburn history is reviewed at every skin exam at Couture Dermatology to contextualise the overall risk profile.
Board-Certified FAAD
Harvard-trained, board-certified Fellow of the American Academy of Dermatology — every skin exam and biopsy performed personally
Dermoscopy at Every Exam
Dermoscopy used at every skin check — improving melanoma diagnostic accuracy by approximately 30% over the unaided eye in trained hands
Biopsy Same Day
No second appointment required — shave, punch, and excisional biopsies performed in-office on the same visit when clinically indicated
9735 Wilshire Blvd, Suite 216
Beverly Hills, CA 90212 · (310) 444-0946 · Mon–Fri 9 AM–6 PM
The Short Answer:
Every Adult. Annually.
What to do between annual skin exams
Monthly self-examination is recommended by the American Academy of Dermatology for all adults. The most effective method is examining your skin in a well-lit room with a full-length mirror, using a hand mirror for areas you cannot see directly — the scalp, upper back, and backs of the legs. Know your moles: most people have 10–40 moles; you should know roughly where they are and what they look like, so that a new lesion or change in an existing one is detectable.
Daily SPF 30 or higher broad-spectrum sunscreen — applied to all sun-exposed skin including the scalp, ears, lips, and the backs of hands — is the most evidence-supported preventive intervention for skin cancer and for premature UV-induced skin ageing. Physical (mineral) sunscreens with zinc oxide and titanium dioxide provide broad-spectrum UVA and UVB protection and are the recommended formulation for daily use on the face.
The Best Outcome Is a
Skin Cancer That Never Progresses.
A thin melanoma caught during a routine annual skin exam requires a wide local excision and carries greater than 95% five-year survival. The same melanoma found two years later, having grown to 4mm thickness, is a stage III cancer requiring sentinel node biopsy, systemic therapy, and carries a profoundly different prognosis. The annual skin exam is not a precaution — it is the most cost-effective intervention in dermatological oncology.
9735 Wilshire Blvd, Suite 216 · Beverly Hills, CA 90212 · Mon–Fri 9 AM–6 PM
Frequently
Asked Questions
Direct answers to the most common questions about skin cancer screening, what the exam involves, and when to be concerned about a mole or lesion.
Annual full body skin exams are recommended for all adults by the American Academy of Dermatology. Patients with elevated risk factors require more frequent monitoring: every 6–12 months for those with a personal history of skin cancer; every 3–6 months for those with a prior melanoma; every 6–12 months for atypical moles or a family history of melanoma; and every 3–6 months for organ transplant recipients. Your dermatologist will recommend the appropriate interval at your first exam.
Dermoscopy uses a handheld lens that magnifies the skin ×10–40 with polarised light, revealing subsurface pigment architecture and vascular patterns invisible to the naked eye. In trained hands, dermoscopy improves melanoma diagnostic accuracy by approximately 30% over unaided inspection and reduces unnecessary biopsies of benign lesions. At Couture Dermatology, dermoscopy is used at every skin examination — it is not an optional add-on.
If a biopsy is clinically indicated, it is performed at the same appointment under local anaesthetic. Shave, excisional, and punch biopsies are all available in-office. The specimen is sent to a dermatopathologist; results are available in 5–7 business days. Your dermatologist contacts you directly with the result and discusses the next step — whether reassurance, a follow-up visit, wide excision, or Mohs surgery referral.
The ABCDE rule covers the visual warning signs of melanoma: Asymmetry (one half does not match the other); Border (irregular, ragged, or blurred edges); Colour (variation within a single lesion — browns, blacks, reds, whites, blues); Diameter (greater than 6mm); and Evolution (any change in size, shape, colour, or new symptoms such as bleeding or itch). Any lesion meeting one or more criteria warrants evaluation. Nodular melanoma and amelanotic melanoma may not follow the classic pattern and can present as a new pink or flesh-coloured nodule.
The three most common skin cancers are basal cell carcinoma (BCC — pearly translucent papule, rarely metastasises but causes local tissue destruction), squamous cell carcinoma (SCC — firm scaly keratotic lesion with approximately 4% metastatic risk, rising in high-risk patients), and melanoma (arises from melanocytes, highest metastatic potential, prognosis strongly correlated with depth at diagnosis). Early detection of all three — when treatment is simple and outcomes are excellent — is the purpose of the annual skin exam.
The highest-risk factors include: prior skin cancer; fair skin, light eyes, and red or blonde hair; significant lifetime UV exposure including tanning bed use; family history of melanoma; atypical moles; organ transplant recipients on immunosuppression (SCC risk elevated up to 250-fold); and a history of blistering sunburns in youth. Southern California's year-round UV environment elevates baseline risk across all populations.

