Eczema Treatment
in Beverly Hills, CA
Couture Dermatology specializes in treating eczema in Beverly Hills, CA, offering expert care for patients of all ages. Our dermatologists provide personalized solutions to relieve itching, redness, and discomfort caused by eczema. With advanced therapies and compassionate support, we help you achieve healthier, more comfortable skin.
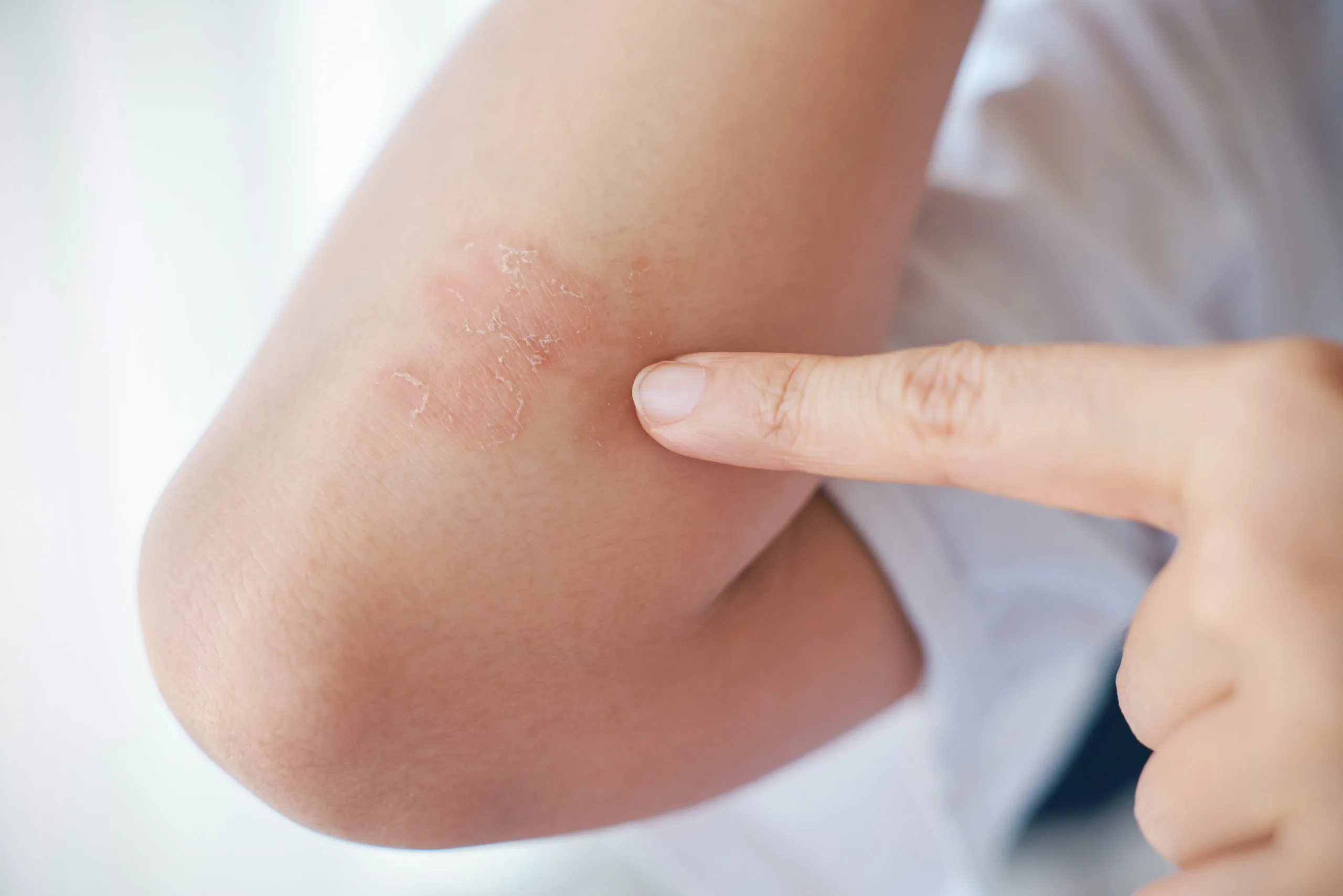
Understanding Eczema
Common Symptoms of Eczema
Intense Itching
Red or Inflamed Skin
Dry or Scaly Patches
Blisters or Oozing Lesions
Thickened or Cracked Skin
Main Causes of Eczema
Eczema Treatment Options
- Topical corticosteroids reduce inflammation and relieve itching.
- Moisturizers help restore the skin barrier and prevent dryness.
- Prescription topical calcineurin inhibitors calm immune responses in the skin.
- Antihistamines can reduce itching and help improve sleep.
- Phototherapy uses controlled UV light to decrease skin inflammation.
- Biologic medications target specific pathways to control severe eczema.
Who Is a Good Candidate?
- Individuals with persistent itching and skin irritation are ideal candidates.
- People experiencing frequent eczema flare-ups benefit from treatment.
- Those who have not found relief with over-the-counter remedies should consider professional care.
- Patients seeking long-term management and improved skin health are good candidates.
Check Your Insurance Coverage
Key Benefits of Eczema Treatment
Reduces Itching and Discomfort
Improves Skin Appearance
Prevents Flare-Ups
Supports Better Sleep Quality
Dr. Chinonso Kagha
Abisogun, MD, FAAD
Why Choose Couture Dermatology for your Eczema Treatment?
Choosing Couture Dermatology means trusting a team of board-certified dermatologists with extensive experience in eczema care. We prioritize a personalized approach, using the latest treatments and technologies to address each patient’s unique needs. Our commitment to compassionate, expert care ensures you receive effective relief and ongoing support for long-term skin health.
Check Your Insurance Coverage
Testimonials

- Rosie D.
Healthy Skin.
Beautiful
Complexion.
A More Confident You.
Eczema & Atopic Dermatitis. Controlled.
Eczema — specifically atopic dermatitis — is a chronic inflammatory skin condition driven by a defective skin barrier and an overactive immune response, not by poor hygiene or an allergen that simply needs to be avoided. The intense, relentless itch that characterises a flare is not incidental; it is the primary clinical burden, disrupting sleep, concentration, and daily life. At Couture Dermatology, eczema management is calibrated to your severity, your skin type, your age, and your flare pattern — from prescription topicals through to biologic therapy for moderate-to-severe disease.
each treated differently
moderate–severe AD
dermatologist

"Eczema is not a hygiene problem or an allergy to be avoided. It is an immune condition that requires clinical management."
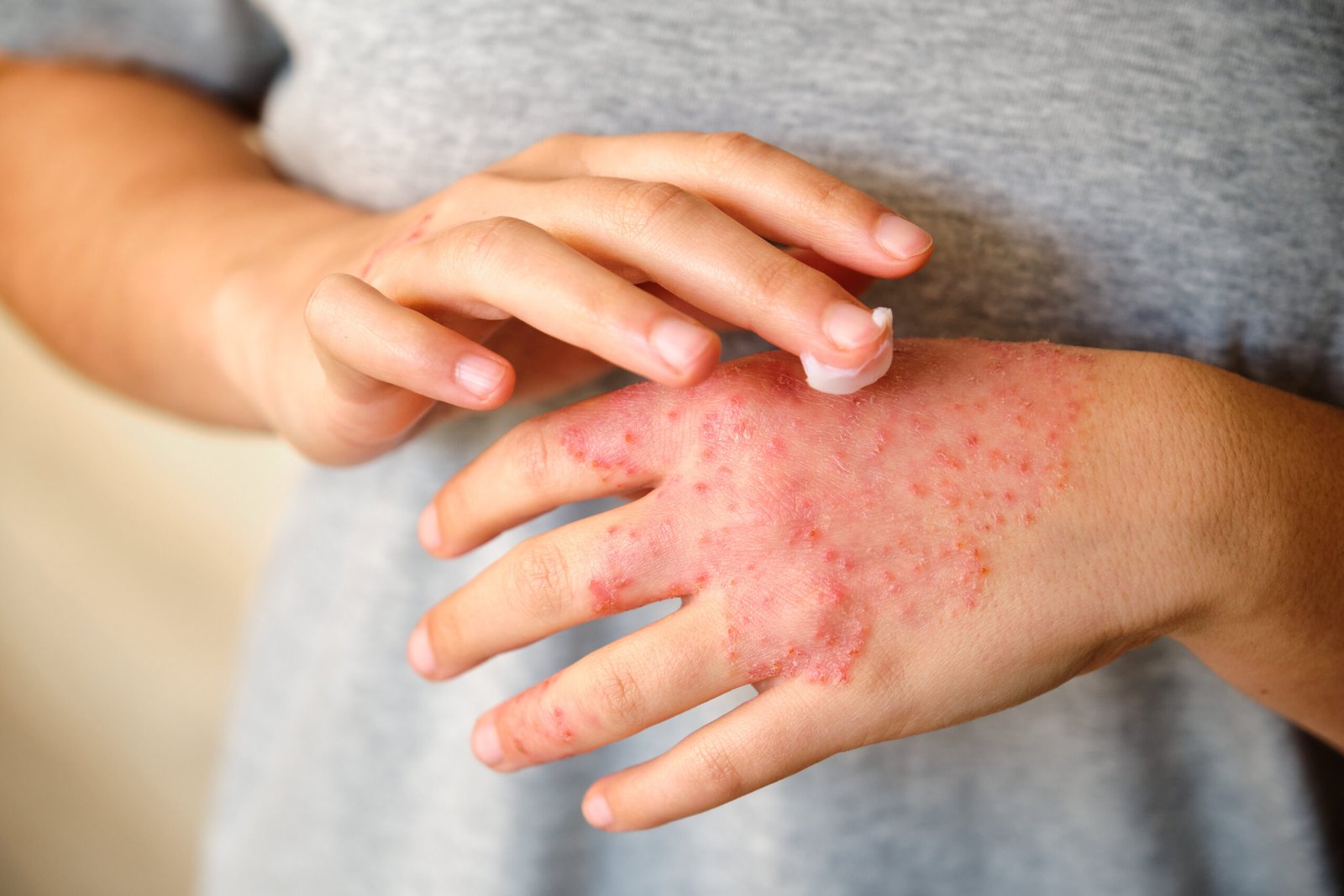
A Barrier and Immune
Condition. Not a Sensitivity.
Atopic dermatitis begins with two co-occurring defects: a compromised skin barrier and an overactive Th2 immune response. The skin barrier in atopic dermatitis has insufficient filaggrin — a structural protein essential for maintaining the tight-junction integrity of the outermost skin layer. Without it, the skin loses water more rapidly (transepidermal water loss), becomes chronically dry, and allows environmental allergens, irritants, and bacteria to penetrate the dermis where they trigger immune activation.
The immune response in atopic dermatitis is skewed toward Th2 cytokines — principally IL-4, IL-13, and IL-31. IL-4 and IL-13 drive the inflammatory cascade that produces the redness, swelling, and weeping of a flare. IL-31 acts directly on sensory neurones, producing the intense pruritus that defines the condition. The itch-scratch cycle is not a habit — it is neurologically driven, and scratching further disrupts the already-defective skin barrier, perpetuating the inflammatory cycle.
This mechanistic understanding is what drives modern eczema treatment: dupilumab targets IL-4 and IL-13 directly; JAK inhibitors suppress the intracellular signalling downstream of these cytokines. Knowing exactly which pathways are overactive explains why these targeted therapies produce outcomes that broad immunosuppressants like ciclosporin — which dampen the immune system indiscriminately — cannot match for safety and durability.
Three Severity Tiers.
Each Treated Differently.
Eczema treatment is not scaled by preference — it is scaled by disease severity and the response to prior therapy. Escalating appropriately, and not over- or under-treating, is the basis of good eczema management.
Limited Areas, Controlled Itch, Manageable Disruption
Mild atopic dermatitis involves dry, itchy skin with occasional areas of redness — typically affecting less than 10% of body surface area. Flares are intermittent and respond promptly to topical treatment. Sleep disruption, if present, is occasional rather than nightly. Mild disease is managed primarily with consistent moisturisation (emollient therapy as the foundation) and short courses of appropriately potent prescription topical corticosteroids during flares — matched to the body site, as potency requirements differ between the face, body folds, and trunk. Over-the-counter hydrocortisone 1% is typically inadequate for managing flares effectively; prescription-strength topical steroids are required.
Widespread Involvement, Frequent Flares, Sleep Disruption
Moderate atopic dermatitis involves more extensive skin involvement — frequently affecting the flexures (inner elbows, behind the knees, wrists, neck), face, and hands — with persistent background redness, lichenification (thickened skin from chronic scratching), and flares that recur within weeks of topical treatment completion. Sleep disruption from nocturnal itch is a defining feature. Topical corticosteroids remain part of the programme but are supplemented with steroid-sparing agents for maintenance use: topical calcineurin inhibitors (tacrolimus 0.1% or pimecrolimus), which are not associated with skin thinning and can be used continuously on sensitive areas including the face and eyelids. Crisaborole (a PDE4 inhibitor) is an alternative steroid-free topical. Patients who do not achieve adequate control with topicals are assessed for systemic therapy.
Extensive Disease, Continuous Itch, Significant Quality of Life Impact
Severe atopic dermatitis involves extensive skin involvement with near-continuous itch, frequent skin infections (particularly Staphylococcus aureus — which colonises atopic skin and perpetuates inflammation), significant sleep disruption, and a quality of life impact comparable to other serious chronic conditions. Topical therapy alone is inadequate for severe disease; systemic treatment is required. Dupilumab — a biologic targeting IL-4 and IL-13 — is the most evidence-supported systemic option, with a well-characterised long-term safety profile and no requirement for routine blood monitoring. JAK inhibitors (upadacitinib, abrocitinib) are oral small-molecule alternatives with rapid onset. Traditional immunosuppressants (ciclosporin, methotrexate) are used where approved biologics are not accessible but require regular monitoring for toxicity.
Assessment Before
Any Prescription Is Written.
Eczema management at Couture Dermatology begins with a full assessment — not with a prescription pad. The distinction between atopic dermatitis and other eczema types (contact dermatitis, dyshidrotic eczema, seborrhoeic dermatitis) is confirmed clinically, because the management of each is different. A diagnosis of contact dermatitis requires patch testing to identify the specific allergen; atopic dermatitis requires severity classification and a treatment programme scaled to that severity.
For patients with established atopic dermatitis who have used over-the-counter treatments without adequate control, the first clinical step is establishing whether topical therapy has been optimised before escalating to systemic treatment. Many patients presenting for specialist care have been using insufficient potency topicals, applying them too infrequently, or using them only during the most acute phase of a flare rather than maintaining suppression through the recovery period.
Where optimised topical therapy is genuinely inadequate for the severity of disease — which it will be for moderate-to-severe atopic dermatitis — your board-certified FAAD dermatologist will discuss systemic therapy options, including dupilumab and JAK inhibitors, with a clear explanation of the evidence, the mechanism, the monitoring requirements, and what you can realistically expect.
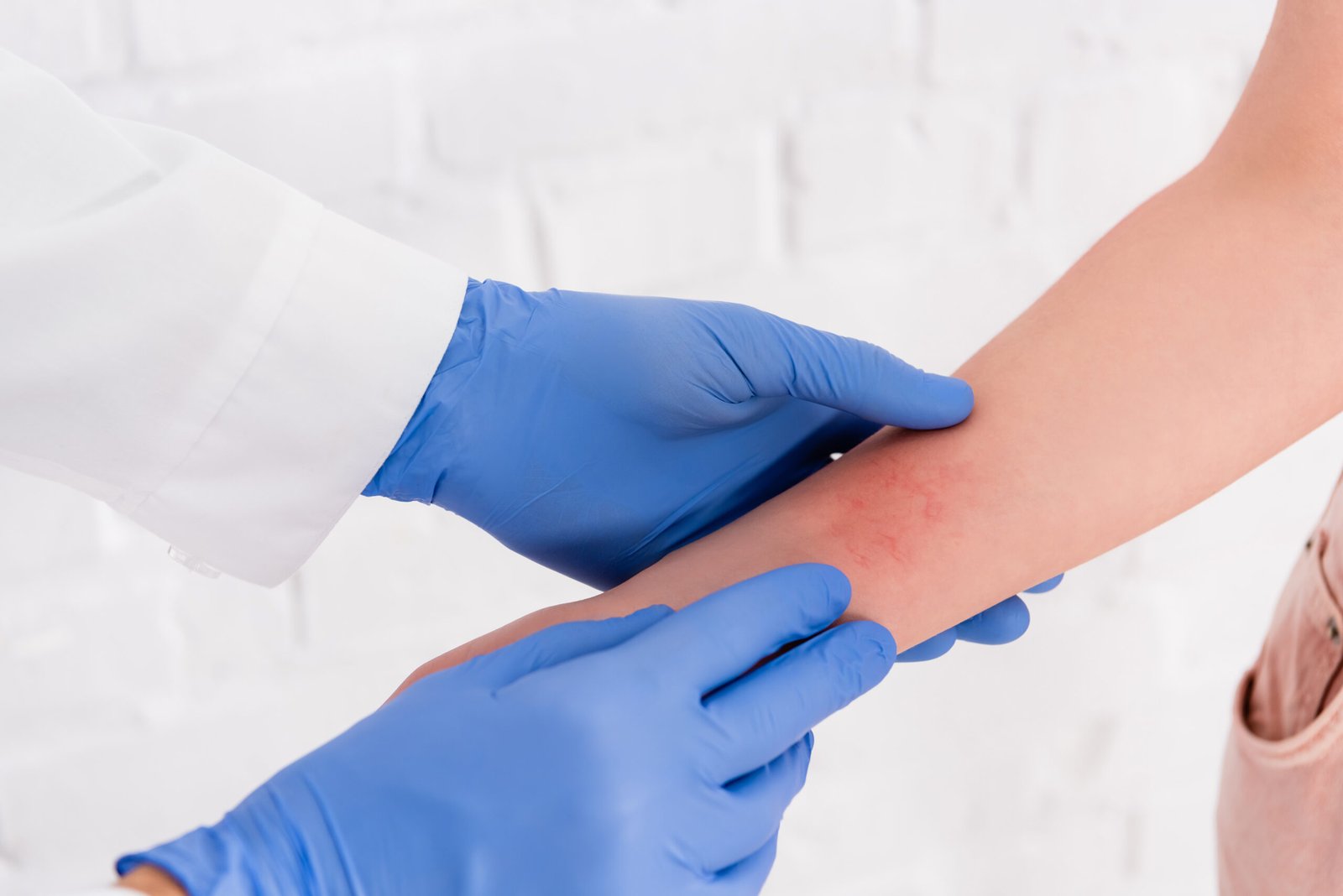
How Eczema Management
Is Structured
Diagnosis & Classification
Your board-certified FAAD dermatologist confirms the eczema type — atopic dermatitis vs contact, dyshidrotic, or seborrhoeic — and classifies severity (mild, moderate, severe) based on body surface area involvement, itch intensity, sleep disruption, and prior treatment response. Staphylococcus aureus colonisation, superinfection, and secondary skin changes (lichenification, excoriation) are assessed. For suspected contact dermatitis, patch testing is arranged.
Included at every visitTrigger Identification
Common triggers are reviewed and a personalised avoidance framework is established: specific soaps and detergents, fabrics (wool, synthetic), fragranced products, dust mite load reduction in the bedroom, pet dander, sweat management, and temperature control. Dietary triggers are relevant only in a subset of young children with confirmed IgE-mediated food sensitisation — routine food elimination in adults with atopic dermatitis is generally not supported by evidence and can cause nutritional harm.
Personalised trigger mapPrescription Treatment
Treatment is selected from the appropriate tier: prescription topical corticosteroids (potency matched to body site and age) and emollient therapy for mild disease; topical calcineurin inhibitors or crisaborole for maintenance and steroid-sparing in moderate disease; dupilumab, JAK inhibitors, or phototherapy for moderate-to-severe disease. Concurrent skin infection is treated before or alongside anti-inflammatory therapy. All prescriptions include clear instructions on application frequency, quantity, and duration.
Scaled to severityMonitoring & Adjustment
Eczema management requires follow-up — not a single prescription. Response to treatment is assessed at 4–8 weeks. For patients on systemic therapy, monitoring is conducted according to the agent: dupilumab requires no routine blood monitoring; JAK inhibitors require periodic laboratory monitoring as per prescribing guidelines. Treatment is adjusted based on response, and step-down is planned proactively when sustained control is achieved rather than maintaining the highest necessary dose indefinitely.
4–8 week follow-upThe Treatments That
Actually Work for Eczema
Modern eczema treatment has progressed enormously — from broad immunosuppression with significant side-effect profiles to targeted biologics that address the specific immune pathways driving atopic dermatitis. Here is what the evidence supports.
Mild–Moderate · First-Line · Anti-Inflammatory
Topical Corticosteroids
Topical corticosteroids remain the first-line treatment for atopic dermatitis flares and the most widely used anti-inflammatory therapy in eczema management. They suppress the local inflammatory response — reducing redness, swelling, itch, and weeping — with onset of effect within 24–48 hours of consistent application. Potency is the most important variable: mild-potency steroids (hydrocortisone 1%) are appropriate only for the face, eyelids, and skin folds in adults, and for children on all sites; moderate- to high-potency steroids (triamcinolone, betamethasone, clobetasol) are required for the body and limbs in moderate-to-severe flares. Using insufficient potency for the site and severity — the most common clinical error — prolongs flares unnecessarily and increases cumulative steroid exposure. Prescription formulations deliver appropriate concentrations; over-the-counter hydrocortisone 1% rarely achieves adequate clinical effect for anything beyond the mildest presentation.
Mild–Moderate · Steroid-Sparing · Maintenance
Topical Calcineurin Inhibitors
Topical calcineurin inhibitors (TCIs) — tacrolimus 0.03% and 0.1%, and pimecrolimus 1% — suppress T-cell activation and the inflammatory cytokine release driving atopic dermatitis without the skin atrophy (thinning) associated with prolonged topical corticosteroid use. This makes them the preferred maintenance treatment for sensitive areas: the face, eyelids, perioral skin, and flexures — sites where topical steroids carry the highest risk of skin thinning with prolonged use. Tacrolimus 0.1% is the more potent formulation (approved for adults); tacrolimus 0.03% is approved for children aged 2 and older. TCIs are used for proactive maintenance therapy — applying 2–3 times weekly to previously affected areas to prevent flares from re-establishing — as well as for active treatment of mild-to-moderate flares in sensitive sites. The historic FDA black box warning for malignancy risk has not been supported by subsequent long-term real-world data, and major dermatology guidelines support their safety for ongoing use.
Moderate–Severe · Biologic · IL-4 / IL-13 Blockade
Dupilumab (Dupixent)
Dupilumab is a fully human monoclonal antibody that blocks the shared IL-4Rα receptor subunit, simultaneously inhibiting IL-4 and IL-13 signalling — the two cytokines central to the Th2 immune dysregulation driving atopic dermatitis. By targeting this specific pathway, dupilumab dramatically reduces skin inflammation, barrier disruption, and the neurogenic itch signal (IL-31 production is also indirectly reduced). Clinical trial data shows 50–80% improvement in EASI (Eczema Area and Severity Index) scores at 16 weeks in patients with moderate-to-severe disease; real-world outcomes are consistent with trials. Dupilumab does not broadly suppress the immune system — it does not increase susceptibility to infections and requires no routine blood monitoring. It is self-administered by subcutaneous injection every two weeks (after an initial loading dose), approved for adults and children aged 6 months and older. The most common side effect is conjunctivitis, reported in approximately 10% of patients — managed with lubricating eye drops or specialist referral. Dupilumab also has approvals for asthma, chronic rhinosinusitis, and food allergies — addressing the atopic march comorbidities that frequently accompany severe atopic dermatitis.
Moderate–Severe · Oral · JAK Inhibition
JAK Inhibitors (Upadacitinib / Abrocitinib)
JAK inhibitors are oral small-molecule therapies that block the JAK-STAT intracellular signalling pathway downstream of multiple cytokine receptors — including those for IL-4, IL-13, IL-31, and TSLP — all of which are overactivated in atopic dermatitis. Upadacitinib (Rinvoq) and abrocitinib (Cibinqo) are both approved for moderate-to-severe atopic dermatitis in adults and adolescents. Their key clinical advantage over dupilumab is speed of onset — meaningful itch reduction is often reported within the first week, compared to 2–4 weeks for dupilumab — making them particularly valuable for patients whose primary burden is uncontrolled itch. They are also effective for patients who have not responded adequately to dupilumab. JAK inhibitors carry a class-wide FDA warning regarding risks of serious cardiovascular events, malignancy, and thrombosis — derived from studies in older patients with rheumatoid arthritis and significant cardiovascular risk factors. For younger, healthy patients with atopic dermatitis, the benefit-risk profile is generally favourable, but requires discussion of individual risk factors at consultation. Routine laboratory monitoring (blood counts, lipid panel) is required during treatment.
Reducing What
Provokes Your Flares
Prescription therapy suppresses active eczema. Trigger management reduces the frequency and severity of new flares. Both are required for the best long-term outcome.
Skin Irritants
Soaps, shower gels, and detergents with surfactants (sodium lauryl sulphate in particular) remove the skin's natural lipid barrier, worsening transepidermal water loss in atopic skin. Fragrance — the most common cause of contact sensitisation — is present in most commercial skincare, laundry products, and cleaning agents. Wool and synthetic fabrics cause mechanical irritation. Switching to fragrance-free, soap-free cleansers and detergents is one of the highest-yield trigger modifications for most eczema patients.
Dry Skin & Insufficient Moisturisation
A defective skin barrier loses water more rapidly than normal skin — transepidermal water loss in atopic dermatitis is measurably elevated even between flares. Emollient therapy is not cosmetic; it is the foundational medical intervention for eczema. Thick creams and ointments (rather than thin lotions) applied within 3 minutes of bathing — while the skin retains water from washing — deliver the most effective barrier repair. Consistent twice-daily emollient use reduces flare frequency measurably in controlled trials.
Staphylococcus aureus Colonisation
Atopic skin is colonised by Staphylococcus aureus at rates far exceeding non-atopic skin. S. aureus produces superantigens that directly activate T cells and exotoxins that trigger IgE-mediated mast cell degranulation — perpetuating the inflammatory cycle independent of other triggers. Dilute bleach baths (sodium hypochlorite 0.005% solution — approximately half a teaspoon of regular bleach per full bath) reduce S. aureus colonisation and are supported by clinical evidence in moderate-to-severe disease. Nasal decolonisation may be recommended where carriage contributes to recurrent skin infections.
Aeroallergens
House dust mite (HDM) is the most consistently identified aeroallergen trigger in atopic dermatitis. HDM allergen contacts the skin surface directly — not just through inhalation — and worsens barrier dysfunction in sensitised patients. Practical HDM reduction: mattress and pillow encasements, washing bedding weekly at 60°C or above, removing carpets from bedrooms, maintaining indoor humidity below 50%. Pet dander (particularly cat) is the second most common aeroallergen trigger; mould and pollen are additional contributors for sensitised individuals.
Heat, Sweat & Temperature
Elevated body temperature and sweating trigger pruritus through direct neural stimulation of C-fibre itch neurones — producing the characteristic exercise-triggered or nighttime itch exacerbation. Keeping the sleeping environment cool (18–20°C), choosing breathable cotton bedding and clothing over synthetic fabrics, and showering promptly after exercise to remove sweat from the skin surface all reduce this trigger. Hot showers (above 38°C) degrade the skin barrier; lukewarm water for bathing is recommended.
Psychological Stress
Psychological stress worsens atopic dermatitis through neuroimmune pathways — cortisol and catecholamine release during stress suppress skin barrier recovery and amplify the inflammatory response. The itch-stress cycle is bidirectional: chronic itch disrupts sleep and causes anxiety, which worsens itch. Where stress is identified as a significant flare trigger, management strategies are discussed at consultation as an adjunct to clinical treatment — not as a replacement for it.
Board-Certified FAAD
Every eczema programme designed by a Harvard-trained, board-certified Fellow of the American Academy of Dermatology with specialist laser fellowship training
Biologic Prescribing
Dupilumab and JAK inhibitors prescribed and monitored in-practice — no referral required for patients who meet criteria for systemic eczema therapy
Paediatric & Adult
Age-appropriate treatment across the full age spectrum — from young children with moderate-to-severe atopic dermatitis through to adults with long-standing disease
9735 Wilshire Blvd, Suite 216
Beverly Hills, CA 90212 · (310) 444-0946 · Mon–Fri 9 AM–6 PM
When to See a
Dermatologist for Eczema
Honest expectations for eczema management
Atopic dermatitis cannot be permanently cured. The underlying genetic predisposition — reduced filaggrin expression, Th2 immune skewing — does not resolve with treatment. What does change, substantially, is the level of disease activity. Modern treatment — particularly dupilumab — can produce skin that is functionally clear, with itch so well-controlled that the condition is not part of daily life. This is a realistic outcome for many patients with moderate-to-severe disease on appropriate systemic therapy.
The most important prognostic factor is treating the right severity with the right tier of therapy. Under-treating moderate-to-severe eczema with mild topical therapy prolongs suffering and drives secondary complications — skin infections, sleep deprivation, psychological impact — that are themselves chronic burdens. Your dermatologist will be direct about whether your current therapy matches your disease severity.
Eczema That Is Finally
Under Control.
If your eczema is not controlled by what you have tried, it is almost certainly a question of whether the treatment matches the severity — not a question of whether effective treatment exists. Modern dermatology has a treatment option for every tier of atopic dermatitis, from optimised topical therapy through to targeted biologic therapy that produces functionally clear skin in the majority of moderate-to-severe patients. The consultation at Couture Dermatology begins with an honest assessment of which tier your disease is at and what you can realistically expect.
9735 Wilshire Blvd, Suite 216 · Beverly Hills, CA 90212 · Mon–Fri 9 AM–6 PM
Frequently
Asked Questions
Direct answers to the questions eczema patients most commonly bring to consultation — on the condition itself, on treatment options, and on what effective management can realistically achieve.
Eczema is a broad umbrella term for several inflammatory skin conditions; atopic dermatitis is the most common and most studied form. When most people say eczema, they mean atopic dermatitis — a chronic, immune-mediated condition driven by a defective skin barrier and Th2-skewed immune response, characterised by intense itch, inflamed skin, and episodic flares. Other forms include contact dermatitis, dyshidrotic eczema, and seborrhoeic dermatitis, each with distinct triggers and management. At Couture Dermatology, the specific type is confirmed before treatment is selected.
Eczema cannot be permanently cured, but it can be very effectively managed. Many children experience significant natural improvement by early adulthood, though flares can recur. Adults with moderate-to-severe disease typically require long-term management. With an appropriate programme — prescription topicals, trigger management, and systemic therapy when indicated — the vast majority of patients achieve sustained periods where eczema is not visibly apparent or significantly disruptive.
Common triggers include dry skin, skin irritants (soaps, detergents, fragranced products, wool), allergens (dust mites, pet dander, certain foods in young children), heat and sweat, stress, and Staphylococcus aureus colonisation. Individual trigger profiles vary significantly. Identifying your primary triggers is discussed at consultation alongside prescription therapy — because trigger avoidance reduces flare frequency while treatment suppresses active disease.
Treatment is calibrated to severity. Mild-to-moderate eczema is managed with prescription topical corticosteroids and topical calcineurin inhibitors (tacrolimus or pimecrolimus — steroid-sparing, suitable for long-term maintenance). Moderate-to-severe disease that does not respond to optimised topicals is treated with dupilumab (biologic, IL-4/IL-13 blockade) or JAK inhibitors (upadacitinib, abrocitinib). Phototherapy is used for extensive disease. All systemic therapies require dermatologist prescribing and monitoring.
Dupilumab (Dupixent) is a biologic that blocks IL-4 and IL-13 — the cytokines central to atopic dermatitis inflammation. It is approved for moderate-to-severe atopic dermatitis from age 6 months and has the strongest long-term safety and efficacy data of any systemic eczema therapy. It is self-injected every two weeks, does not suppress the immune system broadly, and requires no routine blood monitoring. Whether it is appropriate for your disease severity and medical history is assessed at consultation.
Yes — and early effective management matters because poorly-controlled atopic dermatitis in children is associated with the atopic march: the sequential development of allergic rhinitis and asthma. Mild paediatric eczema is managed with emollients and mild prescription topical steroids. Moderate-to-severe disease may require topical calcineurin inhibitors, wet wrap therapy, or dupilumab, which is approved for children aged 6 months and older. Your dermatologist will select age-appropriate therapies at consultation.

