Psoriasis Treatment
in Beverly Hills, CA
Couture Dermatology offers expert care for Psoriasis in Beverly Hills, CA, providing personalized treatment plans to help manage this chronic skin condition. Our experienced dermatologists use advanced therapies to reduce symptoms and improve quality of life. We are committed to supporting you with compassionate care and the latest medical solutions.

Understanding Psoriasis
Common Signs and Symptoms of Psoriasis
Red, Raised Skin Patches
Silvery Scales Formation
Persistent Itching and Discomfort
Cracked or Bleeding Skin
Nail Changes
Primary Causes and Triggers of Psoriasis
Effective Psoriasis Treatment Options
- Topical corticosteroids help reduce inflammation and relieve itching.
- Phototherapy uses controlled ultraviolet light to slow skin cell growth.
- Systemic medications can treat moderate to severe cases from within the body.
- Biologic therapies target specific immune responses causing psoriasis.
- Moisturizers and emollients soothe dryness and help heal the skin barrier.
- Lifestyle modifications such as stress management can minimize flare-ups.
Who Is a Good Candidate
- Individuals experiencing persistent red, scaly skin patches are ideal candidates for psoriasis treatment.
- People whose symptoms interfere with daily comfort or confidence may benefit from treatment.
- Candidates include patients who have not responded to over-the-counter therapies.
- Those with psoriasis-related nail changes or joint pain should consider advanced care.
Check Your Insurance Coverage
Psoriasis Treatment Benefits
Symptom Relief and Comfort
Improved Skin Appearance
Enhanced Quality of Life
Long-Term Health Protection
Dr. Chinonso Kagha
Abisogun, MD, FAAD
Why Choose Couture Dermatology for Psoriasis Treatment
At Couture Dermatology, our board-certified dermatologists offer advanced, individualized care for psoriasis. We utilize the latest therapies and a compassionate approach to help you achieve clearer skin and better symptom control. Our Beverly Hills, CA, clinic is dedicated to supporting your journey with expert guidance and a commitment to lasting results.
Check Your Insurance Coverage
Testimonials

- Rosie D.
Healthy Skin.
Beautiful
Complexion.
A More Confident You.
Psoriasis. Managed to Clearance.
Psoriasis is a chronic immune-mediated inflammatory skin condition driven by T-cell dysregulation — not a skin surface problem, not an allergy, and not a condition that can be resolved with moisturiser. The rapid epidermal cell turnover that produces its characteristic plaques is fuelled by a specific cytokine pathway, and the most effective modern therapies target that pathway precisely. At Couture Dermatology, psoriasis management is calibrated to your subtype, your severity, and your life — from prescription topical therapy through to biologic agents that achieve complete skin clearance in the majority of patients who receive them.
biologic patients
arthritis
dermatologist
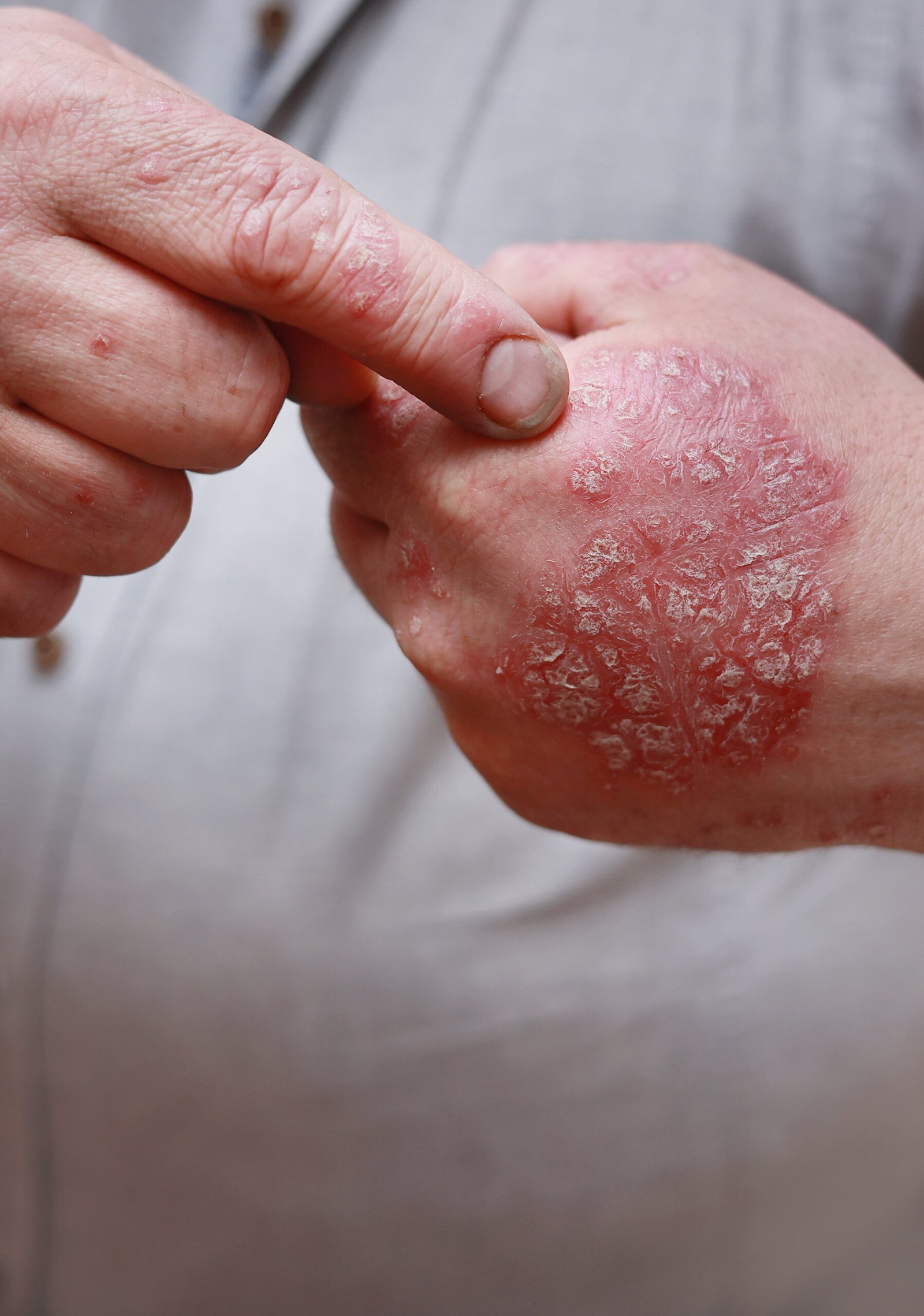
"Modern biologic therapy achieves complete or near-complete skin clearance in the majority of moderate-to-severe psoriasis patients."
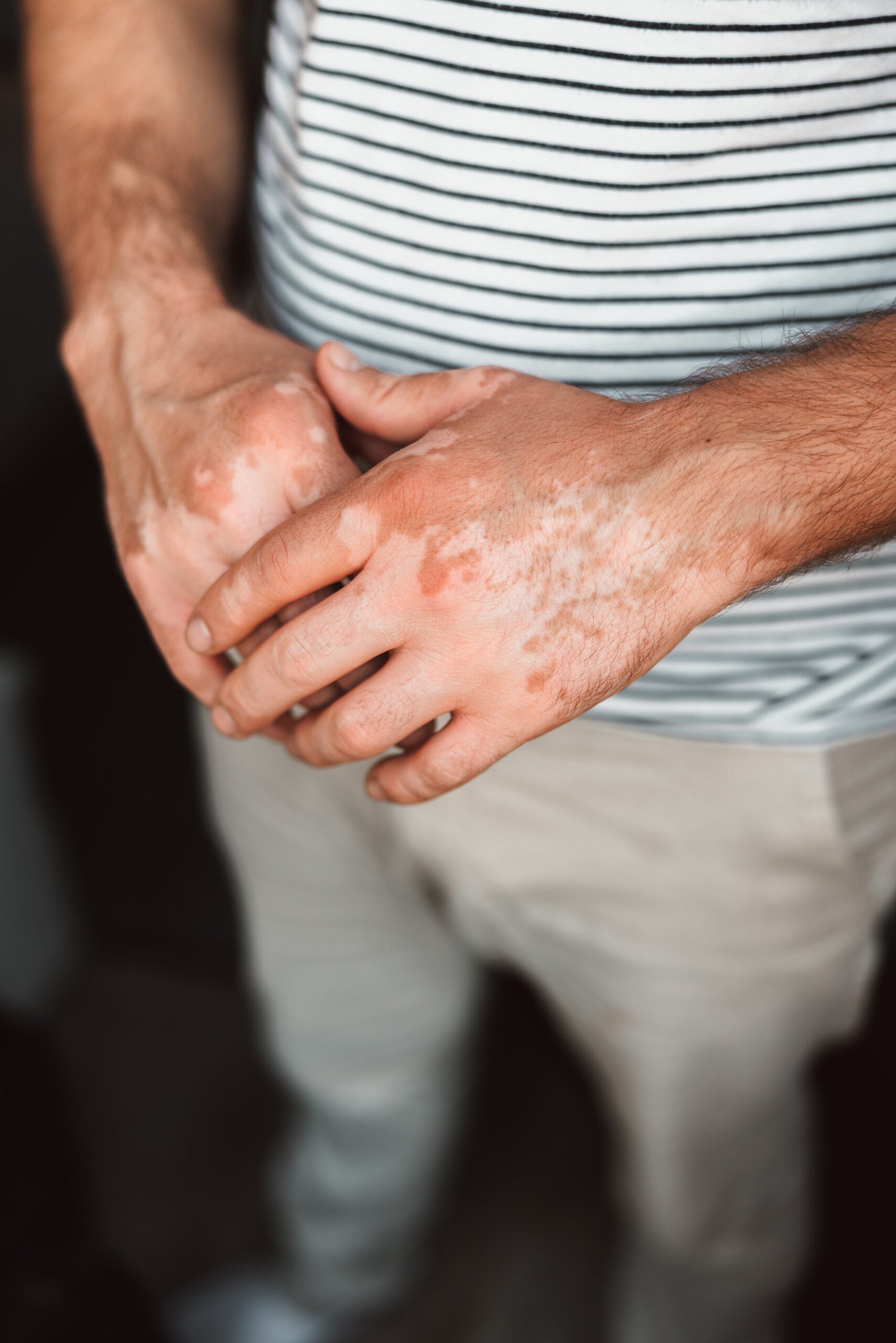
An Immune Condition.
Not a Skin Surface Problem.
Psoriasis begins in the immune system, not in the skin. Activated T-cells — incorrectly recognising skin proteins as foreign — release a cascade of inflammatory cytokines, principally IL-17A, IL-17F, and IL-22, that signal keratinocytes (skin cells) to proliferate at dramatically accelerated speed. In healthy skin, epidermal cells take approximately 28 days to mature and shed from the surface. In psoriasis, this cycle is compressed to 3–5 days — cells accumulate faster than they can shed, producing the characteristic raised, erythematous, silvery-scaled plaques on the surface.
The IL-23/IL-17 axis is the primary driver of this immune dysregulation, which is why the most effective modern therapies — IL-23 inhibitors and IL-17 inhibitors — achieve plaque clearance rates that earlier treatments could not approach. Psoriasis has a strong genetic component: around one-third of patients have a first-degree relative with the condition, and the HLA-Cw6 allele is the strongest known genetic risk factor. But the genetic predisposition alone does not produce disease — environmental triggers activate and perpetuate it.
Psoriasis is also a systemic condition, not confined to the skin surface. Psoriatic arthritis develops in approximately 30% of psoriasis patients; the condition is associated with elevated cardiovascular risk, metabolic syndrome, and inflammatory bowel disease. Managing psoriasis comprehensively means managing it as the systemic inflammatory condition it is — with appropriate screening and, where indicated, cross-specialty coordination.
Five Clinical Subtypes.
Each Presents and Behaves Differently.
Psoriasis subtype determines distribution, severity, trigger pattern, and treatment selection. Most patients have predominantly one subtype, though overlap is common.
Plaque Psoriasis
Psoriasis Vulgaris · 80–90% of CasesThe most common form — well-demarcated, erythematous, raised plaques covered by a silver-white scale. Classic sites are the extensor surfaces: elbows, knees, scalp, and lumbosacral region, though plaques can appear anywhere. Individual plaques range from a few centimetres to extensive confluent involvement covering large body surface areas. Scalp psoriasis — which may extend to the hairline, ears, and nape — is often among the most difficult-to-treat sites due to hair interference with topical application. Plaque psoriasis is chronic and relapsing; it does not spontaneously resolve without treatment and, without management, tends to progress over time. The Koebner phenomenon — new plaques appearing at sites of skin trauma — is characteristic. Disease severity is assessed using the Psoriasis Area and Severity Index (PASI) and body surface area (BSA) involvement.
Guttate Psoriasis
Streptococcal-Triggered · Younger PatientsGuttate psoriasis presents as an acute eruption of small (less than 1cm) drop-shaped scaly papules distributed widely over the trunk and proximal limbs — distinct from the large plaques of psoriasis vulgaris. It is most common in children and young adults and is classically triggered by a streptococcal throat infection, appearing 2–3 weeks after the pharyngitis. The connection to streptococcal infection is well-established: streptococcal superantigens activate T-cells that cross-react with skin keratinocyte antigens, producing the acute eruption. In many patients, guttate psoriasis resolves spontaneously over weeks to months. However, approximately one-third of patients subsequently develop chronic plaque psoriasis. Treatment of the triggering streptococcal infection (if still active) is the first step; phototherapy is effective for the eruption itself.
Pustular Psoriasis
Sterile Pustules · Localised or GeneralisedPustular psoriasis is characterised by sterile pustules — not infected, but filled with neutrophils recruited by the psoriatic inflammatory process — on an erythematous base. It occurs in two principal forms. Localised palmoplantar pustulosis affects the palms and soles, producing crops of yellow-brown pustules that evolve to brown macules and desquamate; it is particularly treatment-resistant. Generalised pustular psoriasis (von Zumbusch type) is an acute, potentially life-threatening form producing widespread sheets of sterile pustules with fever, systemic inflammation, and fluid and electrolyte disturbance requiring urgent hospitalisation and systemic therapy. Triggers include abrupt withdrawal of systemic corticosteroids, pregnancy (impetigo herpetiformis), and certain medications. A new IL-36 receptor inhibitor (spesolimab) is the first biologic specifically approved for generalised pustular psoriasis.
Nail Psoriasis
Pitting · Onycholysis · Subungual HyperkeratosisNail psoriasis occurs in up to 50% of patients with plaque psoriasis and in nearly all patients with psoriatic arthritis — nail involvement is a strong predictor of joint disease and should always prompt screening for arthritis symptoms. The nail matrix produces pitting — small uniform indentations across the nail plate surface. The nail bed produces onycholysis (nail plate separation from the nail bed), subungual hyperkeratosis (thickening of tissue under the nail), and the "oil drop" or "salmon patch" sign — a translucent yellow-brown discolouration visible through the nail plate. Nail psoriasis is one of the most difficult-to-treat manifestations due to poor penetration of topical agents into the nail unit. Systemic therapy — particularly IL-17 inhibitors and methotrexate — produces the most consistent nail improvement.
Erythrodermic Psoriasis
Widespread Erythema · Dermatological EmergencyErythrodermic psoriasis is a rare but severe variant in which erythema and scale involve more than 90% of the body surface area, producing widespread intense redness, warmth, and exfoliation. It is a dermatological emergency — the failure of normal skin barrier function at this extent leads to hypothermia (impaired thermoregulation), fluid and protein loss, secondary infection, and high-output cardiac failure in susceptible individuals. Triggers include abrupt withdrawal of systemic corticosteroids or methotrexate, drug reactions, infection, and severe emotional stress. Management requires urgent hospitalisation, systemic therapy (infliximab, ciclosporin, or acitretin depending on clinical circumstances), supportive care, and monitoring for systemic complications.
Psoriatic Arthritis
Inflammatory Joint Disease · ~30% of Psoriasis PatientsPsoriatic arthritis is an inflammatory joint condition affecting approximately 30% of psoriasis patients — but it is often underdiagnosed because patients attribute joint pain to other causes. It can present in several patterns: oligoarthritis (a few asymmetric joints), polyarthritis resembling rheumatoid arthritis, distal interphalangeal joint involvement (the fingertip joints closest to the nail), sacroiliitis (spinal inflammation), or dactylitis (diffuse swelling of an entire finger or toe — "sausage digit"). Nail psoriasis is the single strongest skin predictor of joint involvement. All psoriasis patients should be routinely screened for musculoskeletal symptoms. Several biologics — TNF inhibitors (adalimumab, etanercept), IL-17 inhibitors (secukinumab, ixekizumab), and IL-23 inhibitors — are approved for both skin and joint disease, enabling coordinated management.
Severity-Matched Treatment.
From Topicals to Biologics.
Psoriasis management follows a well-defined treatment ladder: topical therapy for mild disease; narrowband UVB phototherapy or conventional systemic agents for moderate disease; biologic therapy for moderate-to-severe disease inadequately controlled by other means. The distinction between mild and moderate-to-severe psoriasis is based on body surface area involvement, disease impact on quality of life, and location — psoriasis affecting the palms, soles, nails, genitals, or face is classified as severe regardless of BSA, because these sites have disproportionate quality-of-life impact.
For moderate-to-severe plaque psoriasis, biologic therapy — specifically IL-23 and IL-17 inhibitors — represents the most significant advance in psoriasis treatment in decades. These agents target the specific cytokine pathways driving keratinocyte proliferation with a precision that older systemic therapies (methotrexate, ciclosporin, acitretin) cannot match. PASI 90 response — 90% reduction in disease severity — is achieved in 70–80% of patients on IL-17 inhibitors and in 60–75% of patients on IL-23 inhibitors in clinical trials. Complete clearance (PASI 100) is achieved in a substantial proportion.
At Couture Dermatology, the assessment includes current severity, prior treatment history, comorbidities (particularly psoriatic arthritis, cardiovascular risk, and inflammatory bowel disease — which influence biologic selection), and patient preference regarding injection frequency. All biologic prescribing and monitoring is conducted in-practice.
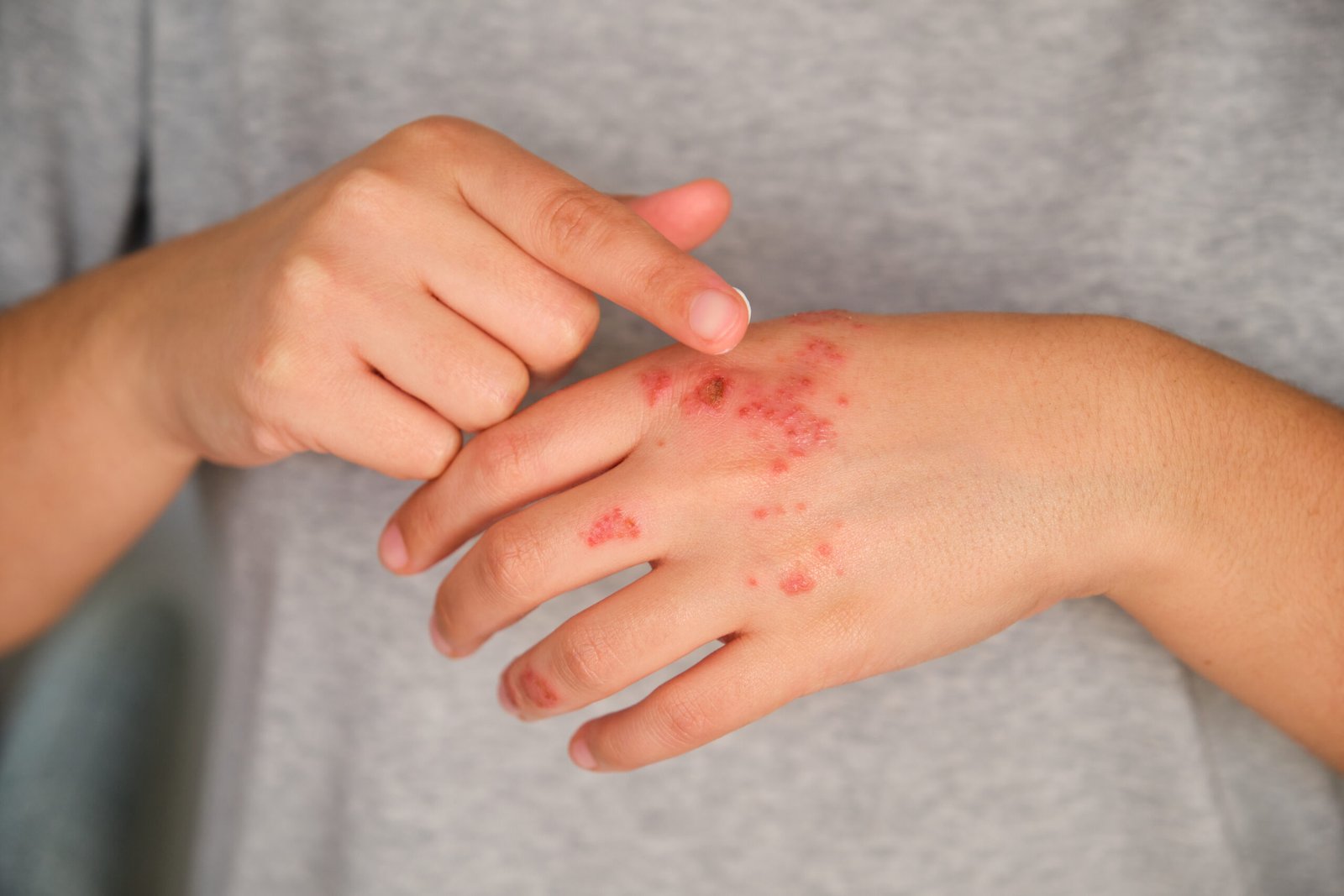
The Options — and What
the Evidence Says About Each
Psoriasis treatment has a well-defined hierarchy of efficacy. These are the principal options, from topical agents through to the most effective biologic therapies currently available.
Mild Disease · First-Line · Topical
Topical Corticosteroids & Vitamin D Analogues
Prescription topical corticosteroids are the cornerstone of mild psoriasis management — suppressing the local inflammatory response to reduce plaque thickness, erythema, and scale. Potency selection is critical: high-potency agents (clobetasol propionate 0.05%, betamethasone dipropionate) are required for the body and limbs; medium-potency for the face and flexures; mild-potency for children and sensitive sites. Topical vitamin D analogues (calcipotriol/calcipotriene) normalise keratinocyte differentiation and reduce proliferation through a complementary mechanism to corticosteroids. Their combination — calcipotriol/betamethasone dipropionate in a single formulation (Taclonex, Enstilar foam) — is the most evidence-supported topical regimen and produces significantly greater plaque clearance than either agent alone. Tazarotene (a topical retinoid) reduces keratinocyte proliferation and is used for stubborn plaques, often in combination with a topical steroid to mitigate local irritation. Topical therapy is effective for limited disease but practically inadequate for moderate-to-severe plaque psoriasis covering large body surface areas.
Moderate Disease · Second-Line · Phototherapy
Narrowband UVB Phototherapy
Narrowband UVB (NB-UVB) phototherapy — delivered at 311–313nm — suppresses the T-cell driven inflammatory response in psoriatic skin through a combination of T-cell apoptosis and immunomodulation, producing plaque clearance across the whole body in a way that topical therapy alone cannot achieve for widespread disease. It is administered 2–3 times per week in-office; a typical course is 20–30 sessions. Response rates for plaque psoriasis are 65–75% achieving PASI 75, making it an effective and low-cost option for moderate disease. Unlike PUVA (psoralen plus UVA), NB-UVB does not require oral photosensitising medication and is safe in pregnancy. Practical limitations are the requirement for frequent clinic visits and the reality that response rates and durability are inferior to biologic therapy for moderate-to-severe disease. NB-UVB is used as monotherapy for moderate disease, in combination with topical therapy or a systemic agent, or as a bridge to biologic therapy.
Moderate–Severe Disease · Targeted · IL-17 Blockade
IL-17 Inhibitors
IL-17 inhibitors — secukinumab (Cosentyx), ixekizumab (Taltz), and bimekizumab (Bimzelx) — are the fastest and most efficacious class of biologics for plaque psoriasis. By directly blocking IL-17A, IL-17F, or both (in the case of bimekizumab), they interrupt the primary downstream effector cytokine that drives keratinocyte hyperproliferation. Clinical trial data demonstrates PASI 90 response in 70–80% of patients at 12–16 weeks, with PASI 100 (complete clearance) achieved in 40–60% depending on the agent. Bimekizumab — the newest IL-17 agent — simultaneously blocks both IL-17A and IL-17F, producing the highest PASI 100 rates in head-to-head trials. These agents are administered by subcutaneous injection on an induction schedule followed by maintenance injections every 4–8 weeks depending on the specific drug. IL-17 inhibitors are also highly effective for psoriatic arthritis. The principal monitoring consideration is candidal infection risk — IL-17 plays a protective role against mucocutaneous candidiasis, and a modest increase in oral or vaginal thrush is reported in approximately 4–5% of patients on IL-17 inhibitors.
Moderate–Severe Disease · Durable · IL-23 Blockade
IL-23 Inhibitors
IL-23 inhibitors — guselkumab (Tremfya), risankizumab (Skyrizi), and tildrakizumab (Ilumya) — act upstream of IL-17 inhibitors, blocking the p19 subunit of IL-23 that is required for the differentiation and survival of the Th17 cells responsible for IL-17 production. By targeting further upstream in the inflammatory cascade, they produce more durable responses with less frequent dosing than IL-17 inhibitors. Risankizumab achieves PASI 90 in approximately 75% of patients at 16 weeks; after the induction phase, maintenance is every 12 weeks — the longest dosing interval of any approved psoriasis biologic. Guselkumab produces PASI 90 in approximately 70% of patients with maintenance dosing every 8 weeks. IL-23 inhibitors have an excellent safety profile — they do not increase candidal infection risk as IL-17 inhibitors do, and their more targeted mechanism allows a favourable profile in patients with inflammatory bowel disease (where IL-17 inhibitors are contraindicated). For patients prioritising infrequent dosing and long-term durability, IL-23 inhibitors are generally preferred.
From First Consultation
to Sustained Clearance
Severity Assessment
Your board-certified FAAD dermatologist assesses psoriasis subtype, body surface area involvement, PASI score, and quality-of-life impact. Nail involvement is documented. Musculoskeletal symptoms — joint pain, morning stiffness, swollen digits — are systematically screened. Special sites (scalp, palms, soles, genitals, face) are noted as they elevate functional severity regardless of BSA. Prior treatment history, current medications, and relevant comorbidities are reviewed before any treatment is selected.
Complete at first visitComorbidity & Arthritis Screening
Psoriatic arthritis is screened using validated tools (PEST questionnaire) and clinical examination. Cardiovascular risk — elevated in moderate-to-severe psoriasis — is discussed and any existing management reviewed. Inflammatory bowel disease history is noted, as it influences biologic selection (IL-17 inhibitors are contraindicated in active IBD; IL-23 inhibitors are safe). Hepatic function is assessed where methotrexate is being considered. Rheumatology referral is coordinated where psoriatic arthritis is confirmed or suspected.
Before biologic prescribingTreatment Selection
Treatment is selected based on severity tier, comorbidities, prior response history, and patient preference regarding injection frequency and route. For mild disease, optimised topical therapy is prescribed with clear application instructions. For moderate-to-severe disease, biologic therapy is discussed — with an honest explanation of the mechanism, the expected response timeline, PASI 90 rates by agent, the monitoring requirements, and what the dosing schedule involves. The patient's informed choice is the basis of the prescribing decision.
Informed patient decisionMonitoring & Adjustment
For patients on biologic therapy, response is assessed at 12–16 weeks — the standard timepoint for clinical trial endpoints. Biologics not producing at least PASI 50 at 16 weeks are reviewed for dose optimisation or switching. Patients achieving PASI 90 or better are maintained on the current agent with periodic follow-up. Pre-biologic tuberculosis screening (IGRA or Mantoux), hepatitis B and C serology, and varicella immunity status are assessed before initiation as per prescribing guidelines. Laboratory monitoring frequency thereafter depends on the specific agent.
12–16 week response assessmentPsoriasis Is a Systemic
Inflammatory Condition.
The inflammation driving psoriasis does not confine itself to the skin. These are the systemic associations that inform how psoriasis should be managed and which biologics are appropriate for each patient.
Psoriatic Arthritis
Affects approximately 30% of psoriasis patients — often presenting years after the skin condition. It can be erosive and destructive without treatment. Nail psoriasis is the single strongest predictor of joint involvement. Early identification and systemic therapy — particularly biologics with joint approvals — prevents irreversible joint damage. All psoriasis patients should be screened for musculoskeletal symptoms at every dermatology visit.
Cardiovascular Disease
Moderate-to-severe psoriasis is an independent cardiovascular risk factor — the chronic systemic inflammation drives atherosclerosis and endothelial dysfunction. The elevated cardiovascular risk in severe psoriasis is comparable to that of type 2 diabetes. Management includes cardiovascular risk factor assessment and discussion of lifestyle modifications alongside dermatological treatment. Effective control of psoriatic inflammation with biologic therapy is associated with reduced cardiovascular event rates.
Metabolic Syndrome
Psoriasis patients have significantly elevated rates of obesity, hypertension, dyslipidaemia, and insulin resistance — collectively metabolic syndrome. The shared inflammatory mechanisms between psoriasis and metabolic disease create a bidirectional relationship: metabolic syndrome worsens psoriasis severity and makes treatment less effective, while systemic psoriatic inflammation promotes metabolic dysregulation. Weight loss in obese psoriasis patients improves biologic response rates and can independently reduce disease severity.
Inflammatory Bowel Disease
Crohn's disease and ulcerative colitis occur at significantly elevated rates in psoriasis patients. The association is mechanistic — shared genetic susceptibility loci and overlapping inflammatory pathways. IBD history is critical to biologic selection: IL-17 inhibitors are contraindicated in active Crohn's disease (they can paradoxically worsen it) and should be used with caution in ulcerative colitis. IL-23 inhibitors are safe and effective in both conditions. Any history of IBD must be disclosed at consultation before biologic therapy is prescribed.
Board-Certified FAAD
Harvard-trained, board-certified dermatologist — every psoriasis programme assessed, prescribed, and monitored personally
Biologic Prescribing In-Practice
IL-17 and IL-23 biologics prescribed and monitored at Couture Dermatology — no external referral required for the most effective psoriasis therapies
Psoriatic Arthritis Screening
Systematic joint screening at every visit — rheumatology referral coordinated where psoriatic arthritis is confirmed or suspected
9735 Wilshire Blvd, Suite 216
Beverly Hills, CA 90212 · (310) 444-0946 · Mon–Fri 9 AM–6 PM
When to See a Dermatologist
for Psoriasis
Honest expectations for psoriasis management
Psoriasis cannot be permanently cured — the underlying genetic predisposition and immune dysregulation do not resolve with treatment. What does change, dramatically, is the level of active disease. For patients with moderate-to-severe plaque psoriasis on an appropriate IL-17 or IL-23 biologic, complete or near-complete skin clearance is a realistic and frequently achieved outcome — not an optimistic projection.
The most important factor in treatment planning is matching the treatment tier to the disease severity. Mild topical therapy applied to moderate-to-severe psoriasis covering large surface areas is an inadequate match that produces inadequate results and prolongs the period of avoidable disease burden. Your dermatologist will assess your severity honestly and discuss the full range of options — including biologic therapy — at consultation.
Psoriasis That No Longer
Defines Your Skin.
Modern biologic therapy has transformed the outlook for moderate-to-severe psoriasis. PASI 90 — skin that is 90% or more clear — is now a realistic and frequently achieved treatment benchmark, not an aspirational endpoint. If your current management is not producing this level of clearance, the consultation at Couture Dermatology begins with an honest assessment of whether you are receiving the most effective therapy available for your disease severity.
9735 Wilshire Blvd, Suite 216 · Beverly Hills, CA 90212 · Mon–Fri 9 AM–6 PM
Frequently
Asked Questions
Direct answers to the questions psoriasis patients most commonly bring to consultation — on the condition's cause, its association with joint disease, and what modern treatment can realistically achieve.
Psoriasis is caused by immune dysregulation — an overactive T-cell response driven by IL-17 and IL-23 signalling that stimulates keratinocytes to proliferate far faster than normal. In healthy skin, epidermal cells take 28 days to mature and shed; in psoriasis, this cycle is compressed to 3–5 days, producing the characteristic scale accumulation. Psoriasis has a strong genetic component, but environmental triggers — stress, streptococcal infection, certain medications, skin trauma, smoking, and alcohol — activate and perpetuate it.
No. Psoriasis is not contagious. It is an autoimmune condition driven by the patient's own immune system — the plaques contain no infectious agent and cannot be transmitted through skin contact or any other route. This is a frequent source of social distress for patients with visible psoriasis; it has zero transmission risk.
Biologics target specific cytokines driving psoriasis inflammation. IL-17 inhibitors (secukinumab, ixekizumab, bimekizumab) and IL-23 inhibitors (guselkumab, risankizumab, tildrakizumab) achieve PASI 90 — 90% reduction in disease severity — in 70–80% of patients with moderate-to-severe disease. They are administered by subcutaneous injection every 2–12 weeks depending on the agent. Whether biologic therapy is appropriate depends on disease severity, prior treatment response, and medical history — assessed at consultation.
Psoriatic arthritis is an inflammatory joint condition affecting approximately 30% of psoriasis patients. It presents as painful, swollen joints — often asymmetric — with morning stiffness, dactylitis (swollen digits), or sacroiliitis. Nail psoriasis is a strong predictor. It can precede, accompany, or follow skin psoriasis. All psoriasis patients are screened for musculoskeletal symptoms at Couture Dermatology. Rheumatology is involved for confirmed cases. Several biologics are approved for both skin and joint disease, allowing coordinated management.
Common triggers include psychological stress (the most consistently identified), streptococcal throat infection (which precipitates guttate psoriasis), certain medications (lithium, beta-blockers, antimalarials, NSAIDs in some patients), skin injury causing the Koebner phenomenon, smoking, and alcohol excess. Identifying and managing your individual triggers is discussed as part of every psoriasis management programme alongside prescription therapy.
Psoriasis cannot be permanently cured — the genetic predisposition does not resolve with treatment. However, it can be managed to a state of minimal or no visible disease. Modern biologic therapy — IL-17 and IL-23 inhibitors — produces complete or near-complete skin clearance in the majority of moderate-to-severe patients. The goal at Couture Dermatology is skin that does not limit daily life, comfort, or confidence — which is achievable for most patients with the current therapies available.

