Hair Loss Treatment
in Beverly Hills, CA

Understanding Hair Loss
Common Signs of Hair Loss
Gradual Thinning on Top
Sudden Loosening of Hair
Patchy or Circular Bald Spots
Full-Body Hair Loss
Scalp Redness or Scaling
Leading Causes of Hair Loss
Effective Treatments for Hair Loss
- Topical medications can help stimulate hair regrowth and slow thinning.
- Oral medications may address underlying causes and promote healthier hair.
- Platelet-rich plasma (PRP) therapy uses your own growth factors to encourage new hair growth.
- Low-level laser therapy can improve hair density and strength.
- Microneedling enhances scalp health and supports hair regeneration.
- Hair transplant procedures offer lasting solutions for significant hair loss.
Who Qualifies for Treatment
- Adults experiencing noticeable hair thinning or shedding.
- Individuals with patchy bald spots or receding hairlines.
- Patients seeking medical or cosmetic solutions for hair loss.
- Those with stable health and realistic expectations for results.
Check Your Insurance Coverage
Benefits of Hair Loss Treatment
Restores Natural Hair Growth
Boosts Confidence and Self-Esteem
Personalized, Advanced Solutions
Improves Scalp Health
Dr. Chinonso Kagha
Abisogun, MD, FAAD
Why Choose Couture Dermatology for your Hair Loss Treatment?
Couture Dermatology stands out for its expert team, personalized approach, and commitment to using the most advanced hair loss treatments. Our Beverly Hills, CA, dermatologists carefully assess each patient’s unique needs, ensuring a customized treatment plan for optimal results. With a focus on compassionate care and proven techniques, we help you restore your hair and confidence.
Check Your Insurance Coverage
Testimonials

- Rosie D.
Healthy Skin.
Beautiful
Complexion.
A More Confident You.
Hair Loss & Alopecia. Diagnosed. Treated.
Hair loss is not a single condition — it is a symptom with a dozen distinct causes, each requiring a different treatment approach. Androgenetic alopecia responds to anti-androgen therapy. Alopecia areata requires immunomodulation, with FDA-approved JAK inhibitors now achieving scalp coverage in patients who had no effective systemic option until 2022. Telogen effluvium requires identifying and correcting the underlying trigger. Scarring alopecias require early diagnosis to halt irreversible follicle destruction. At Couture Dermatology, hair loss is assessed by type before any prescription is written.
each treated differently
systemic therapy for AA
dermatologist
"Hair loss is a symptom, not a diagnosis. The right treatment depends entirely on which type of alopecia is causing it."

The Wrong Treatment
for the Wrong Type Achieves Nothing.
Minoxidil applied to alopecia areata may produce minimal benefit. Finasteride prescribed to a woman with telogen effluvium from iron deficiency will not address the shedding. Aggressive scalp treatments applied to an active scarring alopecia can worsen irreversible follicle damage. The treatment of hair loss is entirely dependent on which condition is producing it — and the only way to determine that is clinical assessment by a dermatologist who specialises in hair and scalp disease.
Hair loss is measured in three dimensions: the pattern of loss (where on the scalp and how it distributes), the type of hair shed (miniaturised hairs vs full-thickness telogen hairs vs broken hairs at the scalp surface), and the timeline of onset (gradual over years, sudden over weeks, or episodic with periods of stability). These three variables — pattern, type, and timeline — combined with the examination of the scalp surface under dermoscopy (trichoscopy) produce the diagnosis that determines treatment selection.
At Couture Dermatology, the assessment includes trichoscopy of the scalp, targeted blood tests selected for the clinical picture (not a blanket panel applied to every patient), a full medication and health history review, and where indicated, a scalp biopsy to confirm a suspected scarring alopecia diagnosis before committing to long-term immunosuppressive therapy.
Six Types of Hair Loss.
Six Different Treatment Approaches.
These are the most common alopecia diagnoses seen in dermatology practice. Each has a distinct cause, clinical presentation, and treatment approach.
Androgenetic Alopecia
Male & Female Pattern Hair Loss · Most CommonAndrogenetic alopecia (AGA) is the most common form of hair loss — affecting approximately 50% of men by age 50 and 40% of women by age 70. It is driven by the action of dihydrotestosterone (DHT) on genetically susceptible hair follicles: DHT binds androgen receptors in the follicle, shortening the anagen (growth) phase with each successive hair cycle and progressively miniaturising the follicle until it no longer produces visible hair. In men, this produces the characteristic bitemporal recession and vertex thinning described by the Norwood-Hamilton scale. In women, it produces diffuse thinning over the crown with preservation of the frontal hairline — described by the Ludwig scale — and does not typically result in complete baldness. Female AGA is frequently associated with hormonal factors including elevated androgens (PCOS), post-menopausal oestrogen decline, and androgenic oral contraceptives. The earlier treatment is started, the more follicular function can be preserved — existing miniaturised follicles can regain function with treatment, but follicles that have been completely lost cannot be restored with medication.
Alopecia Areata
Autoimmune · Patchy to Complete Hair LossAlopecia areata (AA) is an autoimmune condition in which CD8+ T-cells invade the hair follicle in response to a breakdown of the immune privilege that normally protects follicular antigens from immune recognition. The T-cells attack the follicle, pushing it prematurely into the resting (telogen) phase and producing sudden, typically non-scarring patchy hair loss in coin-shaped circular areas. Trichoscopy of the affected scalp shows characteristic "exclamation mark" hairs at the patch margin. AA occurs across all ages and ethnicities. It exists on a severity spectrum: patchy AA (one or a few patches, most common); alopecia totalis (complete scalp hair loss); alopecia universalis (complete scalp and body hair loss). Spontaneous regrowth occurs in some cases, particularly with limited patchy disease, but complete scalp hair loss has a poor prognosis without treatment. Baricitinib (2022) and ritlecitinib (2023) are the first FDA-approved oral systemic treatments for severe AA.
Telogen Effluvium
Diffuse Shedding · Trigger-Driven · Often ReversibleTelogen effluvium (TE) occurs when a physiological shock pushes a large proportion of anagen (growing) hairs simultaneously into the telogen (resting) phase. Two to four months later — the duration of the telogen phase — these hairs shed simultaneously, producing the sudden, alarming, and diffuse hair shedding that characterises TE. The triggering events include major illness (including COVID-19, where telogen effluvium is now well-documented in the post-acute phase), significant surgery, childbirth (postpartum TE — the most common form, occurring 2–4 months after delivery), severe psychological stress, rapid weight loss, crash diets, and nutritional deficiency. In acute TE, hair regrows spontaneously within 6–12 months once the trigger resolves. In chronic TE (persisting beyond 6 months), an ongoing metabolic trigger is almost always present: iron deficiency is the most common culprit, even at serum ferritin levels in the low-normal range — many trichologists use a ferritin threshold of 50–70 µg/L rather than the standard laboratory reference range for hair cycling. Thyroid dysfunction (both hypothyroid and hyperthyroid) is the second most common reversible cause.
Lichen Planopilaris
Scarring Alopecia · Lymphocytic · Permanent if UntreatedLichen planopilaris (LPP) is the most common primary scarring (cicatricial) alopecia — a lymphocytic inflammatory condition that targets the stem cell niche at the base of the hair follicle, producing follicle destruction and replacement with fibrosis. Unlike non-scarring alopecias, the hair loss in LPP is permanent in areas where the follicle has been destroyed — hair cannot regrow in scarred zones. The scalp shows patchy alopecia with the characteristic perifollicular erythema and scale — redness and scaling precisely at the follicle opening — and a violaceous border at the active margin. Trichoscopy is invaluable in active LPP. Symptoms include scalp burning, itching, and tenderness at the active margins. Frontal fibrosing alopecia (FFA) is a variant of LPP producing progressive recession of the frontal and temporal hairline with characteristic loss of eyebrows, eyelashes, and facial follicles — particularly common in postmenopausal women. Early diagnosis and treatment to halt the inflammatory process is critical; treatment does not restore hair already lost but prevents further irreversible scarring.
Central Centrifugal Cicatricial Alopecia
Scarring · Crown-Origin · Most Common in Black WomenCentral centrifugal cicatricial alopecia (CCCA) is the most common scarring alopecia in women of African descent. It begins at the crown of the scalp and spreads centrifugally — from the centre outward — producing a patch of permanently scarred alopecia that expands progressively without treatment. Symptoms include scalp tenderness, burning, and pruritus, though some patients are asymptomatic. Trichoscopy shows peripilar white-grey halos around follicles — a specific finding. The pathogenesis is multifactorial: genetic predisposition (PADI3 gene variants are associated), combined with potential contributions from heat, chemical relaxers, and traumatic hairstyling practices producing traction on the follicle — though CCCA occurs in patients with no history of relaxers or heat styling, indicating genetics are the primary driver. Scalp biopsy is often required for definitive diagnosis. Treatment aims to halt scarring progression; as with all scarring alopecias, lost follicles cannot be restored.
Traction Alopecia
Mechanical · Reversible Early · Permanent if ChronicTraction alopecia results from chronic tension on the hair follicle — from tight braids, cornrows, weaves, ponytails, buns, extensions, or headbands worn daily over months to years. The sustained mechanical traction produces follicular inflammation and, if continued, progressive miniaturisation and ultimately permanent follicle destruction along the hairline and margins. It is particularly prevalent in women who wear protective hairstyles with high tension at the hairline. Early traction alopecia — presenting as perifollicular erythema and papules at the hairline without scarring — is reversible: removing the traction allows follicular recovery and hair regrowth. Late traction alopecia with established scarring is not. The clinical distinction between early and late traction alopecia on trichoscopy determines the prognosis and shapes the urgency of the intervention. In early disease, the single most effective treatment is hairstyle modification to eliminate tension — within a clinically structured conversation about hair practices and cultural context.
Blood Tests, Trichoscopy,
and Scalp Biopsy When Needed.
The investigation of hair loss is targeted to the clinical suspicion, not a one-size panel applied to every patient. For diffuse shedding consistent with telogen effluvium, the minimum investigation includes serum ferritin (iron stores), thyroid function (TSH and free T4), full blood count for anaemia, zinc, and vitamin D. In women, hormonal assessment may include DHEAS, testosterone, free androgen index, SHBG, and prolactin — particularly where there are other features of hyperandrogenism or where PCOS is suspected.
Trichoscopy — dermoscopy of the scalp at high magnification — is performed at every hair loss assessment. In androgenetic alopecia it reveals hair shaft diameter variability: miniaturised thin hairs interspersed among normal-calibre hairs, with a ratio of miniaturised hairs greater than 20% considered a diagnostic threshold. In alopecia areata it shows exclamation mark hairs, yellow dots (empty follicle openings), and black dots (broken hairs). In scarring alopecias it reveals follicular destruction, fibrosis, and the characteristic perifollicular changes specific to each subtype.
Where a scarring alopecia is suspected and the diagnosis is uncertain, or where committing to long-term immunosuppressive therapy requires histological confirmation, a scalp punch biopsy is performed in-office under local anaesthetic. The biopsy is taken from the active inflammatory margin — not the scarred centre — and is read by a dermatopathologist experienced in hair pathology. Results direct the treatment decision.
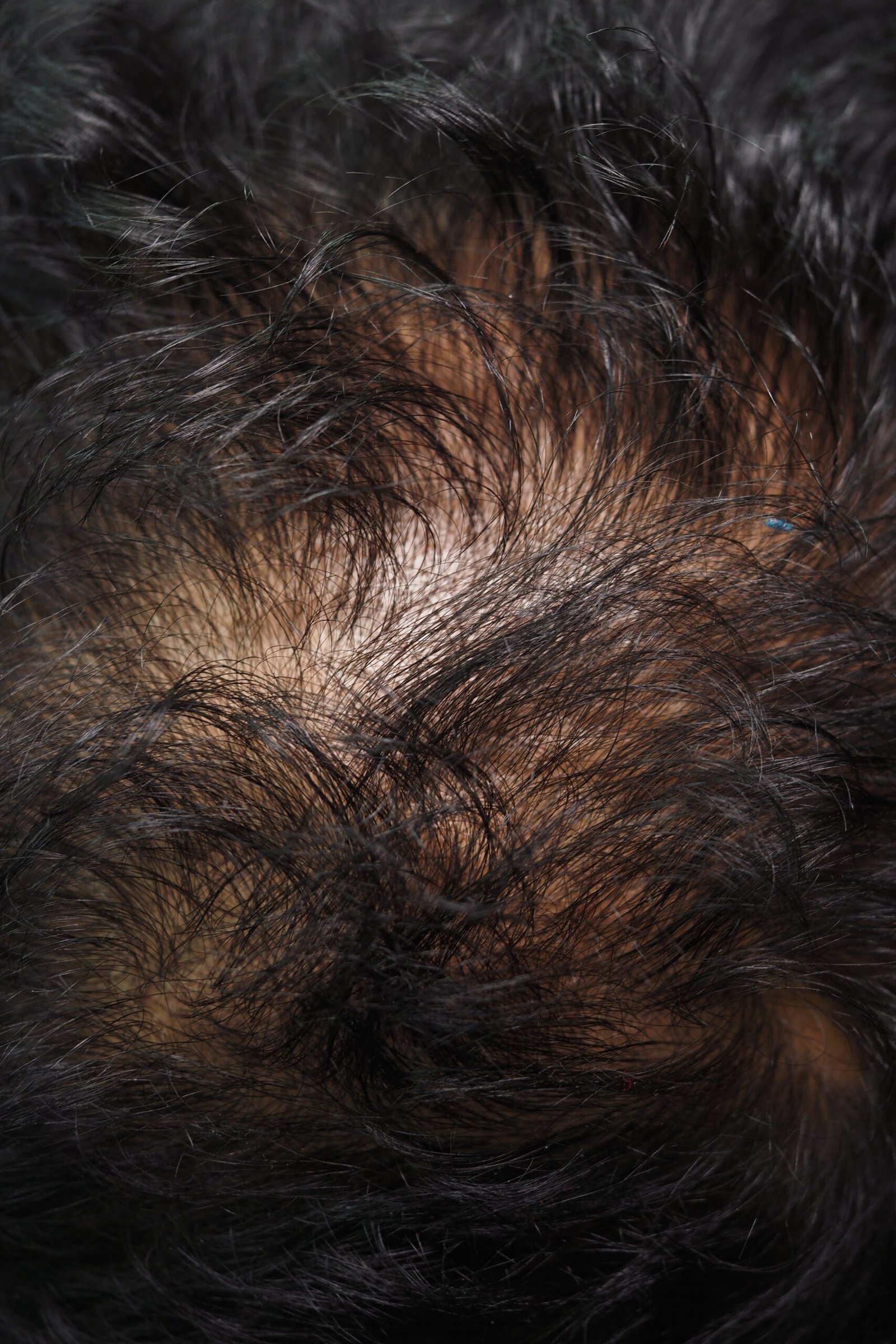
The Treatments — and What
Each Actually Does
Each treatment approach is specific to a hair loss type. These are the principal medical treatments used at Couture Dermatology, with the mechanism and evidence behind each.
Androgenetic Alopecia · First-Line · Anti-Androgen
Minoxidil & Finasteride
Minoxidil is a potassium channel opener that prolongs the anagen (growth) phase of the hair cycle and stimulates follicular proliferation through mechanisms that include increasing VEGF expression and opening ATP-sensitive potassium channels in follicular dermal papilla cells. Topical minoxidil 5% (twice daily) and oral low-dose minoxidil (0.25–2.5mg daily in women; 2.5–5mg in men) are both effective for androgenetic alopecia with similar efficacy — oral minoxidil is gaining preference for better adherence. It does not address the underlying DHT-mediated miniaturisation; it supports existing follicle function but does not stop the genetic programme. Finasteride (1mg daily) inhibits 5-alpha reductase type II, blocking the conversion of testosterone to DHT — targeting the mechanism driving AGA directly. It reduces scalp DHT by approximately 60% and produces statistically significant improvement in hair count and thickness in the majority of men treated over 12–24 months. Dutasteride (0.5mg daily) inhibits both 5-alpha reductase type I and II, reducing DHT by approximately 90%, and produces superior results to finasteride in clinical trials — used where finasteride response is suboptimal. All treatments must be continued indefinitely — stopping produces loss of the benefit gained within 6–12 months.
Female Pattern Hair Loss · Anti-Androgen · Hormonal
Spironolactone
Spironolactone is an aldosterone antagonist that competitively blocks androgen receptors in the hair follicle — reducing the effect of DHT and other androgens on follicular miniaturisation without reducing circulating androgen levels. It is the most commonly prescribed anti-androgen for female androgenetic alopecia in the United States, typically at doses of 50–200mg daily. Response is slow and typically requires 6–12 months of continuous therapy before meaningful hair density improvement is apparent. It must not be used in pregnancy — reliable contraception is required for women of reproductive age. Side effects include menstrual irregularity (which generally settles after the first 3 months), breast tenderness, and, at higher doses, postural hypotension. Spironolactone is particularly effective in women with clinical or biochemical evidence of hyperandrogenism — elevated DHEAS, testosterone, or free androgen index — but produces benefit in a significant proportion of women with androgenetic alopecia regardless of measurable androgen elevation, as follicular androgen sensitivity varies independently of circulating levels.
Alopecia Areata · FDA-Approved 2022–2023 · Oral Daily
JAK Inhibitors (Baricitinib / Ritlecitinib)
JAK inhibitors represent the first FDA-approved systemic therapies specifically for alopecia areata — a condition that, until 2022, had no approved medical treatment despite affecting approximately 2% of the population. Alopecia areata is driven by IFN-γ and IL-15 signalling that activates CD8+ T-cells via the JAK1/JAK2 and JAK3 pathways, collapsing the immune privilege of the hair follicle and producing follicular attack. Baricitinib (Olumiant 2mg and 4mg) blocks JAK1 and JAK2, interrupting the IFN-γ driven T-cell activation. In the pivotal BRAVE-AA trials, approximately 35–40% of patients with severe alopecia areata (baseline SALT score ≥50) achieved ≥80% scalp coverage (SALT ≤20) at 36 weeks on baricitinib 4mg — a clinically meaningful response threshold that prior systemic therapies rarely reached consistently. Ritlecitinib (Litfulo 50mg) preferentially blocks JAK3 and TEC family kinases and is approved for patients aged 12 and older — the first approved therapy for adolescents with severe AA. Both agents are oral daily tablets. Suitability requires assessment of disease severity, prior treatment history, tuberculosis screening (IGRA), and relevant comorbidities. Monitoring includes periodic blood count and lipid panel.
Alopecia Areata · Patchy Disease · In-Office
Intralesional Corticosteroid Injections
Intralesional corticosteroid injections — triamcinolone acetonide (2.5–10mg/mL) injected directly into the dermis of alopecia areata patches — suppress the local T-cell inflammatory infiltrate attacking the follicle, allowing follicular recovery and hair regrowth within 4–8 weeks in responsive patches. They are the standard first-line treatment for limited patchy alopecia areata with few discrete patches, producing regrowth in the majority of treated areas with a course of monthly injections. Practical limitations include the requirement for clinic visits, the discomfort of multiple injections per session, and the inability to treat extensive disease affecting large scalp areas (where the volume of injections required is not practical). For patients with more than 4–6 patches or involving more than 25–30% of the scalp, oral systemic therapy (JAK inhibitors or short-course systemic corticosteroids for acute rapid loss) is more appropriate. Scalp atrophy at injection sites is a potential adverse effect; it is minimised by appropriate dilution and injection technique and is generally reversible.
From First Appointment
to Confirmed Diagnosis & Treatment Plan
Clinical History
Your board-certified FAAD dermatologist takes a structured hair loss history: onset, rate of progression, pattern, and whether there has been any spontaneous regrowth. Medication review — any new drugs in the preceding 6 months, including supplements and hormonal contraceptives. Nutritional history and any recent rapid weight change. Family history of hair loss and pattern. Recent significant stressors, illness, or childbirth. Hairstyling practices including heat, chemical processing, and traction. Symptoms of scalp inflammation: itching, burning, and tenderness at the scalp surface.
Thorough at first visitTrichoscopy
The scalp is examined under dermatoscopy (trichoscopy) at ×20 and ×70 magnification. The density of follicular units, hair shaft diameter variability, the proportion of miniaturised hairs, follicle openings, pericapillary changes, and vascular patterns are all assessed. Trichoscopy is non-invasive and provides diagnostic information that clinical examination alone cannot — including distinguishing active from inactive disease in scarring alopecias, and identifying the characteristic patterns specific to each alopecia subtype. Photographic documentation of the trichoscopy findings provides a baseline for monitoring treatment response over time.
Non-invasive in-officeTargeted Investigations
Blood tests are ordered based on the clinical picture — not a blanket panel applied to every patient regardless of presentation. For suspected telogen effluvium: ferritin, thyroid function, FBC, zinc, vitamin D, and B12. For suspected female AGA or hyperandrogenism: DHEAS, testosterone, free androgen index, SHBG, prolactin. Where autoimmune conditions are associated with AA: ANA, thyroid antibodies. A scalp punch biopsy is arranged where the diagnosis is uncertain or where histological confirmation is required before committing to systemic therapy for a suspected scarring alopecia.
Targeted, not blanketTreatment & Monitoring
Treatment is prescribed for the confirmed diagnosis — not the most common diagnosis in the patient's demographic. Response is monitored with repeat trichoscopy and standardised scalp photography at 3–6 monthly intervals. For patients on JAK inhibitors for alopecia areata, the response threshold of SALT ≤20 (at least 80% scalp coverage) is used as the clinical benchmark. For AGA patients on minoxidil and anti-androgens, stabilisation of loss is the initial goal; regrowth follows over 12–24 months of continuous therapy. Treatment plans are adjusted based on response, tolerability, and patient preference.
3–6 monthly follow-upBoard-Certified FAAD
Harvard-trained, board-certified Fellow of the American Academy of Dermatology — every hair loss assessment, diagnosis, and treatment programme conducted personally
JAK Inhibitor Prescribing
Baricitinib and ritlecitinib — the first FDA-approved systemic therapies for severe alopecia areata — prescribed and monitored in-practice for eligible patients
Trichoscopy & Biopsy In-Office
Trichoscopy performed at every hair consultation; scalp punch biopsy available in-office for suspected scarring alopecias requiring histological confirmation
9735 Wilshire Blvd, Suite 216
Beverly Hills, CA 90212 · (310) 444-0946 · Mon–Fri 9 AM–6 PM
When to See a Dermatologist
for Hair Loss
Honest expectations for hair loss treatment
Hair loss treatment is slow. Minoxidil and anti-androgens for androgenetic alopecia require 6–12 months of consistent use before meaningful density improvement is measurable. JAK inhibitors for severe alopecia areata require 36 weeks before the clinical trial benchmarks are assessed. Patience and adherence are the variables most within a patient's control.
The most important distinction in hair loss is whether the follicle is still present and recoverable, or whether it has been permanently destroyed. Non-scarring alopecias — androgenetic alopecia, alopecia areata, and telogen effluvium — affect follicles that can recover with appropriate treatment. Scarring alopecias destroy follicles permanently. This is why early diagnosis in suspected scarring alopecia is not optional — every month of active inflammation that goes untreated is additional permanent loss that no medical treatment can reverse.
Hair Loss That Finally
Has a Diagnosis.
Most hair loss that has not improved with over-the-counter products is either the wrong diagnosis, the wrong treatment for the right diagnosis, or a condition requiring prescription-grade or systemic therapy available only from a dermatologist. The consultation at Couture Dermatology begins with trichoscopy, targeted blood tests, and a full history — producing an accurate diagnosis and a treatment plan matched to what is actually driving the hair loss.
9735 Wilshire Blvd, Suite 216 · Beverly Hills, CA 90212 · Mon–Fri 9 AM–6 PM
Frequently
Asked Questions
Direct answers to the questions hair loss patients most commonly ask — on the distinction between types, the evidence for treatments, and what a dermatology assessment actually involves.
Androgenetic alopecia (AGA) is a genetically programmed miniaturisation of follicles driven by DHT — gradual, progressive, and following predictable patterns (temporal recession in men; diffuse crown thinning in women). Alopecia areata is autoimmune — T-cells attack the follicle producing sudden patchy circular hair loss or, in severe forms, complete scalp or body hair loss. The distinction determines treatment entirely: AGA is managed with anti-androgens (finasteride, minoxidil, spironolactone); alopecia areata with immunomodulatory therapy (intralesional corticosteroids, JAK inhibitors).
Telogen effluvium is diffuse sudden shedding that occurs when a physiological shock — illness, surgery, childbirth, severe stress, rapid weight loss, or nutritional deficiency — pushes hairs into the resting phase simultaneously. Shedding becomes noticeable 2–4 months later. In acute TE, hair regrows spontaneously within 6–12 months once the trigger resolves. In chronic TE (beyond 6 months), an ongoing trigger — most commonly iron deficiency or thyroid dysfunction — must be identified and corrected. Blood tests are the first step.
Yes — baricitinib (approved 2022) and ritlecitinib (approved 2023) are the first FDA-approved systemic treatments specifically for alopecia areata. In clinical trials, approximately 35–40% of patients with severe disease achieved at least 80% scalp coverage after 36 weeks on baricitinib — a meaningful response in patients who previously had no effective systemic option. Ritlecitinib is approved from age 12. Both are oral daily tablets. Suitability requires assessment of severity, prior treatment, and individual medical factors at consultation.
Finasteride is not generally prescribed for premenopausal women due to pregnancy risk. For postmenopausal women with AGA, it is sometimes used off-label. Spironolactone — an androgen receptor blocker — is the more commonly used anti-androgen for female AGA and is better studied in this population. Topical minoxidil 5% and oral low-dose minoxidil are first-line for most women with AGA, with spironolactone added where there is hyperandrogenism or inadequate response.
Investigations are targeted to the clinical picture. For diffuse shedding: serum ferritin, thyroid function (TSH, free T4), full blood count, zinc, vitamin D, and B12. For women with AGA or suspected hyperandrogenism: DHEAS, testosterone, free androgen index, SHBG, and prolactin. Not every test is appropriate for every patient — the dermatologist selects investigations based on the clinical presentation and history, not a blanket panel.
Scarring alopecias destroy the hair follicle and replace it with fibrosis — producing permanent hair loss in affected areas. The most common forms are lichen planopilaris, frontal fibrosing alopecia, and central centrifugal cicatricial alopecia. Hair cannot regrow in scarred zones. Early diagnosis and treatment to halt the inflammatory process is critical — treatment stops further scarring but cannot restore hair already lost. Any scalp symptoms (burning, itching, tenderness) alongside hair loss should be assessed urgently for this reason.

