Skin Rashes Treatment
in Beverly Hills, CA
Couture Dermatology provides expert care for skin rashes in Beverly Hills, CA, helping patients find fast relief and answers. Our board-certified dermatologists diagnose and treat a wide range of rashes, using advanced techniques to address your specific skin concerns. We are dedicated to restoring your skin’s health and comfort with personalized solutions.
Healthy Skin.
Beautiful
Complexion.
A More Confident You.
Skin Rashes. Diagnosed First.
A rash is not a diagnosis — it is a symptom. Contact dermatitis, drug reactions, urticaria, viral exanthems, psoriasis, and eczema can all produce redness, itch, and inflammation that looks superficially similar but requires an entirely different treatment approach. Applying the wrong treatment to the wrong rash delays resolution and can worsen the condition. At Couture Dermatology, every rash is assessed, classified, and diagnosed before any prescription is written — including patch testing in-practice for suspected allergic contact dermatitis.
each managed differently
for contact dermatitis
dermatologist
"A rash is a symptom, not a diagnosis. The right treatment depends entirely on which condition is producing it."
Not All Rashes
Are the Same Condition.
The word "rash" describes an appearance, not a disease. Red, itchy, inflamed skin can be produced by a T-cell mediated immune reaction to a metal in a watchband, by a drug started three weeks ago, by a viral infection, by a mite infestation, or by a chronic inflammatory dermatosis that will recur indefinitely without ongoing management. The clinical assessment that distinguishes between these — the distribution on the body, the morphology of individual lesions, the timeline of onset, the associated symptoms, and the patient history — is what makes dermatological diagnosis different from guessing.
Treating an allergic contact dermatitis with topical steroids without identifying and eliminating the allergen will suppress the rash temporarily and allow it to return as soon as treatment stops. Treating a drug rash with antihistamines while continuing the offending medication achieves nothing. Treating urticaria as eczema, or psoriasis as a non-specific rash, delays the appropriate therapy by months. The investment in correct diagnosis is an investment in treatment that actually works.
At Couture Dermatology, the assessment includes a full history — recent medications, occupational and household exposures, travel, contact with sick individuals, new products, dietary changes — alongside clinical examination of the rash morphology. Patch testing for suspected allergic contact dermatitis is performed in-practice.
Six Common Rash Categories.
Each Requires a Different Approach.
These are the most common rash types seen in dermatology practice. They can look similar at a glance — but the diagnosis, treatment, and prognosis are distinct for each.
Allergic Contact Dermatitis
Immune-Mediated · Delayed HypersensitivityAllergic contact dermatitis (ACD) is a Type IV delayed hypersensitivity reaction — the immune system becomes sensitised to a specific allergen and mounts a T-cell mediated inflammatory response on re-exposure, typically 48–96 hours after contact. The rash appears precisely at the site of contact with the allergen: a watch strap causing wrist eczema (nickel), a fragrance causing facial or neck rash, a rubber glove causing hand dermatitis. Once sensitised, a patient can react to minute quantities of the allergen indefinitely. Common allergens include nickel, fragrance mix, methylisothiazolinone (a preservative in many skincare and household products), colophonium (found in sticking plasters), and rubber accelerators. Patch testing is the only reliable method of identifying the specific sensitiser.
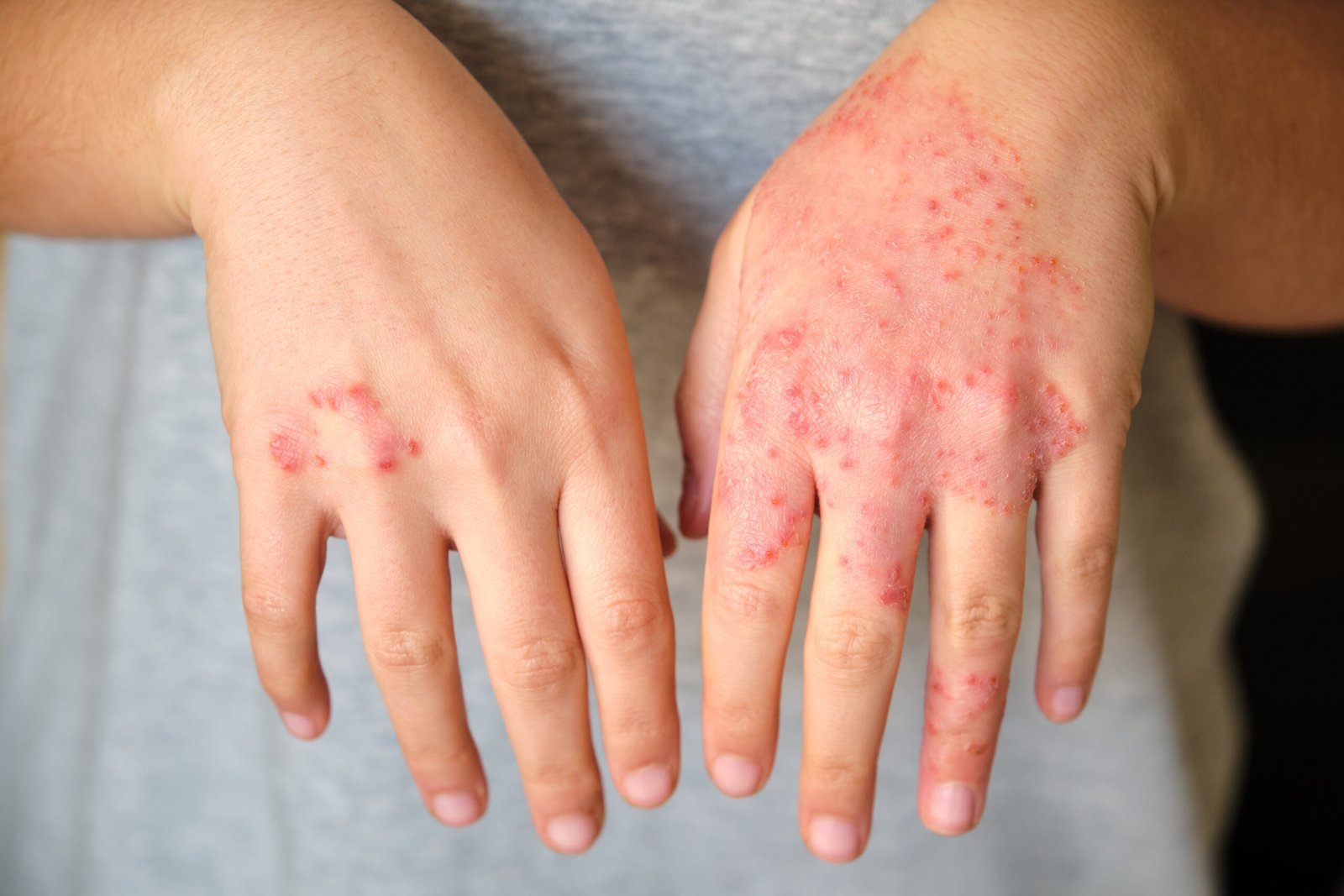
Irritant Contact Dermatitis
Non-Immune · Barrier DisruptionIrritant contact dermatitis (ICD) occurs when a substance directly damages the skin barrier without any immunological involvement. Unlike ACD, it is not specific to a sensitised individual — anyone exposed to sufficient concentration and duration will develop it. Common causes include repeated hand washing (occupational dermatitis in healthcare workers, chefs, hairdressers), detergents and solvents, harsh cleansers, and prolonged water exposure. ICD typically produces a dry, chapped, cracked, or erythematous appearance rather than the vesicular pattern of ACD. The distribution follows the exposure pattern — the hands and forearms for occupational ICD. Management centres on eliminating or minimising the irritant exposure, intensive barrier repair with emollients, and prescription topical therapy for active inflammation.
Drug Rash (Exanthem)
Medication-Induced · Variable SeverityDrug-induced rashes are among the most common adverse drug reactions. The classic morbilliform (measles-like) drug exanthem — widespread symmetrical red spots beginning on the trunk and spreading to the limbs — typically appears 7–14 days after starting the offending medication and fades within 1–2 weeks of stopping it. Common culprits include amoxicillin and other penicillins, cephalosporins, trimethoprim-sulphamethoxazole, allopurinol, and anti-epileptic drugs (lamotrigine, carbamazepine, phenytoin). Drug rashes must be distinguished from the severe cutaneous adverse reactions (SCARs) — Stevens-Johnson Syndrome (SJS), Toxic Epidermal Necrolysis (TEN), and DRESS syndrome — which present with systemic involvement, fever, blistering, and mucous membrane lesions, and require urgent hospitalisation. Any drug rash with these features must be evaluated the same day.
Urticaria (Hives)
Transient Wheals · Acute or ChronicUrticaria is characterised by transient, intensely itchy wheals — raised, pale-centred, red-bordered swellings — that resolve within 24 hours at any individual site, though new lesions continuously appear elsewhere. Acute urticaria (lasting under 6 weeks) is usually triggered by infection, a food allergen, NSAIDs, or a drug; a specific trigger is identified in most acute cases. Chronic urticaria (persisting beyond 6 weeks) is idiopathic in 80–90% of cases — no identifiable trigger despite investigation. Angioedema — deeper swelling involving the lips, tongue, face, or throat — may accompany urticaria and requires prompt assessment when throat involvement is present. Treatment is with second-generation antihistamines (cetirizine, loratadine, fexofenadine) taken regularly, not just on demand. Chronic urticaria uncontrolled by high-dose antihistamines is treated with omalizumab — a biologic with established efficacy in this setting.
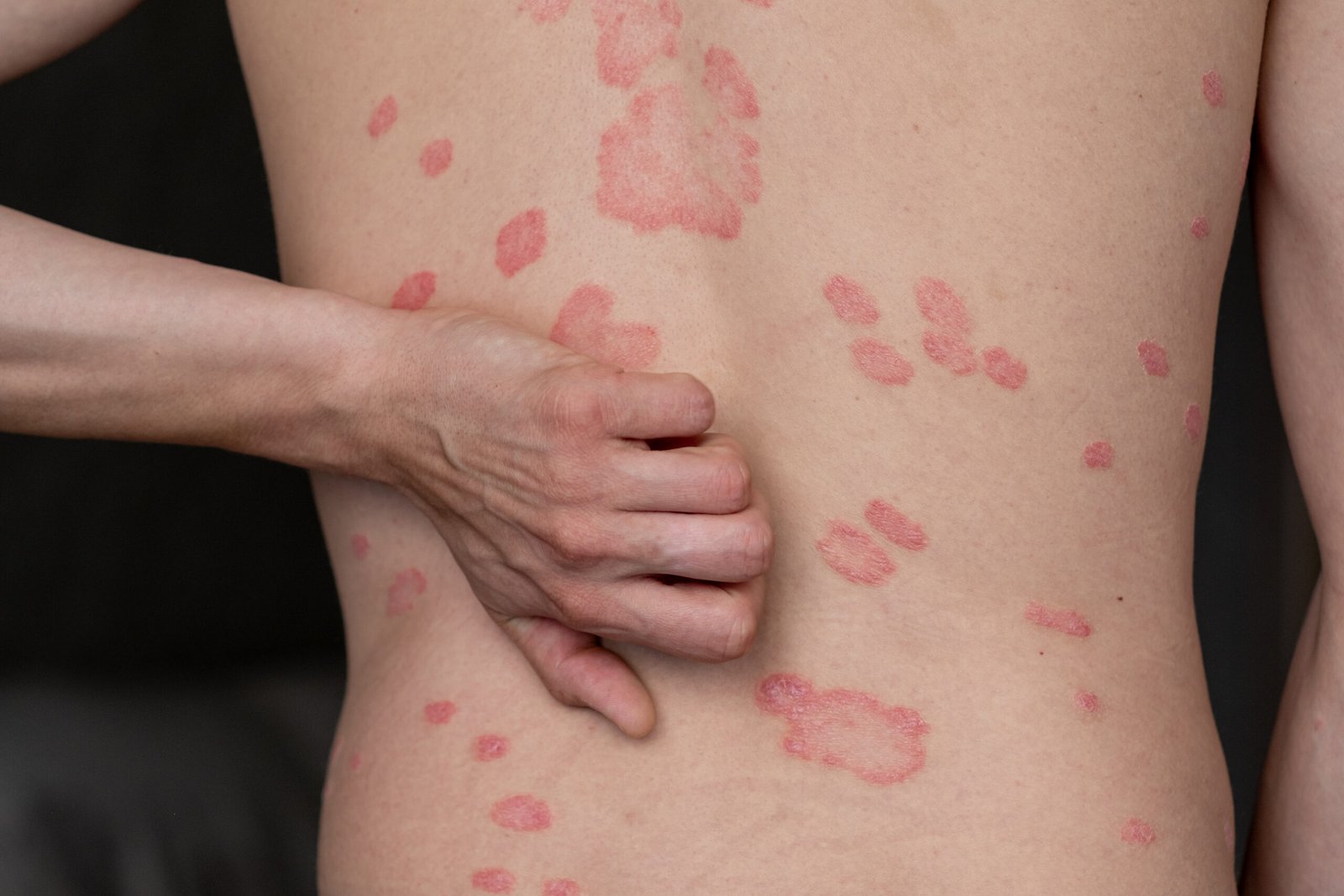
Pityriasis Rosea
Viral-Triggered · Self-LimitingPityriasis rosea is a self-limiting viral exanthem — typically associated with human herpesvirus 6 or 7 reactivation — characterised by an initial single oval "herald patch" on the trunk followed 1–2 weeks later by a widespread eruption of smaller oval scaly patches following the lines of the ribs in a "Christmas tree" distribution on the back. It is most common in young adults, resolves spontaneously over 6–12 weeks, and does not recur. The rash causes itch in approximately 50% of patients; topical corticosteroids and oral antihistamines provide symptomatic relief. The importance of diagnosing pityriasis rosea correctly is to avoid unnecessary investigation and treatment — and to reassure patients that it will resolve. Secondary syphilis, which can look very similar, must be excluded in sexually active patients.
Lichen Planus
Immune-Mediated · Pruritic Purple PapulesLichen planus is an immune-mediated inflammatory dermatosis classically producing the 4 Ps: Pruritic, Purple, Polygonal, Papules — typically on the flexor wrists, ankles, and lower back, often with a fine white surface network (Wickham's striae). It can also affect the mucous membranes (oral lichen planus, producing a white reticular pattern on the inner cheeks), the nails, and the scalp (lichen planopilaris — a scarring alopecia). Cutaneous lichen planus typically resolves over 1–2 years, though oral and scalp variants can be chronic. Management is with potent topical corticosteroids, topical calcineurin inhibitors for mucosal disease, and systemic therapy (hydroxychloroquine, acitretin, or ciclosporin) for extensive or refractory disease.
Finding the Allergen
That Is Driving the Rash.
Patch testing is the gold-standard diagnostic investigation for allergic contact dermatitis and is performed in-practice at Couture Dermatology. A standard allergen panel — covering the most common contact sensitisers including metals (nickel, cobalt, chromate), fragrances, preservatives, rubber chemicals, topical medicaments, and occupational allergens — is applied to the upper back in small aluminium chambers (Finn chambers) and left in place for 48 hours.
The chambers are removed at 48 hours and the back is read for reactions — any localised eczematous response at an allergen site is recorded. The back is read again at 96 hours, as some allergens (particularly metals and corticosteroids) produce late reactions that are not apparent at the 48-hour read. A positive reaction at a specific allergen site confirms that substance as a sensitiser for that patient.
The clinical relevance of each positive result is then determined — a positive reaction to a preservative is only clinically relevant if that preservative is present in a product the patient uses. Identifying the allergen is the first step; identifying its hidden sources in everyday products the patient has not connected to their rash is the second, and often more demanding, step. Your dermatologist will work through the specific relevance of each positive result and provide a personalised avoidance guide.
From First Appointment
to Confirmed Diagnosis
History & Assessment
Your board-certified FAAD dermatologist takes a detailed history — onset and duration, distribution and progression of the rash, associated symptoms (itch, pain, fever, joint involvement), recent medications (including new medications started in the preceding 6 weeks), occupational and household chemical exposures, new skincare or personal care products, recent travel, and contact with individuals who are unwell. The rash is examined for morphology — the appearance of individual lesions — and distribution pattern, which together narrow the diagnostic possibilities considerably.
Thorough at first visitDifferential Diagnosis
Based on the history and examination, a differential diagnosis is established — the ranked list of most likely conditions producing the clinical picture. For many rashes, the clinical assessment is sufficient to confirm the diagnosis. Where contact allergen involvement is suspected, patch testing is arranged. Where a drug reaction is possible, the offending medication is identified and discussed. Where secondary syphilis, dermatomyositis, or systemic causes must be excluded, appropriate investigations are ordered.
Before any prescriptionPatch Testing (Where Indicated)
For suspected allergic contact dermatitis, patch testing is scheduled. Allergen chambers are applied to the upper back and left in place for 48 hours — patients are advised to avoid getting the area wet and to minimise physical activity during this period. The back is read at 48 hours (chambers removed) and again at 96 hours. Results are discussed at the 96-hour visit with a full explanation of the clinical relevance of each positive result and a personalised allergen avoidance guide.
48h + 96h appointmentsTargeted Treatment
Treatment is prescribed based on the confirmed diagnosis. For contact dermatitis, allergen avoidance is the primary intervention — prescription topical therapy manages active inflammation while the allergen is eliminated. For urticaria, regular antihistamines and trigger management. For drug rashes, discontinuation of the offending agent. For inflammatory dermatoses (lichen planus, psoriasis, eczema), appropriate prescription therapy scaled to severity — including systemic options where the clinical picture warrants.
Matched to confirmed diagnosisRashes That Cannot
Wait for a Routine Appointment.
Most rashes are uncomfortable but not dangerous. These presentations are exceptions — they require same-day or emergency evaluation. If in doubt, seek urgent care.
Rash with Difficulty Breathing or Throat Tightening
Urticaria with throat or airway involvement indicates anaphylaxis — a life-threatening emergency requiring immediate epinephrine (adrenaline) and emergency services. Do not drive yourself. If you have a prescribed epinephrine auto-injector (EpiPen), use it and call 911. This is not a situation for an antihistamine alone.
Non-Blanching Purpuric Rash with Fever
Small red-purple spots or blotches that do not turn white when pressed (non-blanching) accompanied by fever, headache, or stiff neck may indicate meningococcal disease or vasculitis. This is a medical emergency. Call 911 or go directly to an emergency department — do not wait for a dermatology appointment.
Rapidly Spreading Blistering Rash with Skin Pain
A painful, rapidly spreading rash with blistering, skin detachment, fever, and involvement of the eyes, mouth, or genitals may indicate Stevens-Johnson Syndrome (SJS) or Toxic Epidermal Necrolysis (TEN) — severe drug reactions requiring immediate hospitalisation and specialist care. Typically associated with a medication started in the preceding 1–8 weeks.
Drug Rash with Fever, Lymph Node Swelling & Internal Organ Involvement
DRESS syndrome (Drug Reaction with Eosinophilia and Systemic Symptoms) presents as an extensive rash with fever, facial oedema, enlarged lymph nodes, and involvement of internal organs — liver, kidneys, lungs. It develops 2–8 weeks after starting the offending drug and requires prompt hospitalisation. Anti-epileptic drugs and allopurinol are common causes.
Board-Certified FAAD
Every rash evaluated by a Harvard-trained, board-certified Fellow of the American Academy of Dermatology with specialist diagnostic and laser training
Patch Testing In-Practice
Allergen patch testing for allergic contact dermatitis performed and read in-practice — no external referral required for the most common diagnostic investigation for chronic contact rashes
Diagnosis Before Prescription
No prescription is written before the diagnosis is established — the correct treatment depends entirely on which condition is producing the rash
9735 Wilshire Blvd, Suite 216
Beverly Hills, CA 90212 · (310) 444-0946 · Mon–Fri 9 AM–6 PM
Signs Your Rash Needs
a Dermatologist
What to bring to your appointment
The more information your dermatologist has about the rash history, the more efficiently the diagnosis can be reached. Consider noting: exactly when the rash first appeared and whether it is new or recurrent; all medications you are currently taking, including over-the-counter and supplements; any new products introduced in the weeks before the rash appeared (skincare, detergent, cleaning products, personal care); your occupation and any chemical exposures at work; recent travel, illness, or contact with unwell individuals; anything that makes the rash better or worse.
If you have tried any treatments — topical or oral — note what you used, for how long, and what effect it had. A rash that partially responds to topical steroids but returns is a different clinical picture to one that does not respond at all.
The Right Diagnosis.
The Right Treatment.
Most rashes that have not improved with over-the-counter treatments are either the wrong diagnosis, the wrong treatment for the right diagnosis, or a condition requiring prescription-grade therapy that is only available from a dermatologist. A 30-minute consultation at Couture Dermatology covers the full history, clinical assessment, and — where indicated — an investigation plan that includes in-practice patch testing. The result is a diagnosis and a treatment that actually addresses the underlying cause.
9735 Wilshire Blvd, Suite 216 · Beverly Hills, CA 90212 · Mon–Fri 9 AM–6 PM
Frequently
Asked Questions
Direct answers to the most common questions patients bring to consultation about skin rashes — on what causes them, when to worry, and how they are diagnosed and treated.
See a dermatologist if your rash has persisted for more than 2 weeks without improvement; if it is spreading, worsening, or involving the face; if it is associated with fever or systemic symptoms; if over-the-counter treatments have not helped; if you suspect a drug reaction; or if the rash recurs repeatedly at the same location. Many rashes that look similar require very different treatments — an accurate diagnosis is the most important step.
Irritant contact dermatitis (ICD) occurs when a substance directly damages the skin barrier — detergents, solvents, and repeated water exposure cause ICD without any immune involvement. Anyone exposed sufficiently will develop it. Allergic contact dermatitis (ACD) is an immune-mediated delayed reaction to a specific allergen — the immune system becomes sensitised and reacts on re-exposure 48–96 hours later. ACD can be triggered by tiny amounts and requires patch testing to identify the specific allergen.
Patch testing is the gold-standard test for allergic contact dermatitis. A standard panel of common allergens is applied to the upper back in small chambers and left for 48 hours. The patches are removed and the back is read at 48 hours then again at 96 hours — looking for localised eczematous reactions at individual allergen sites. A positive reaction confirms that allergen as a sensitiser. Patch testing must be performed by a dermatologist — over-the-counter scratch tests and blood tests do not reliably identify contact allergens.
Yes — drug reactions are among the most common causes of sudden widespread rashes. The classic morbilliform drug rash — widespread symmetrical red spots — appears 7–14 days after starting the offending drug and fades after stopping it. Common culprits include penicillins, cephalosporins, sulphonamides, anti-epileptic drugs, and allopurinol. Rare but severe drug reactions (SJS, TEN, DRESS) present with blistering, fever, and systemic involvement and require immediate emergency evaluation.
Urticaria (hives) produces transient, intensely itchy wheals that resolve within 24 hours at any individual site. Acute urticaria (under 6 weeks) is usually triggered by infection, food, or a drug. Chronic urticaria (over 6 weeks) is idiopathic in 80–90% of cases. Treatment is with regular second-generation antihistamines (cetirizine, loratadine). Chronic urticaria not controlled by antihistamines is treated with omalizumab — a biologic with established efficacy. Urticaria with throat swelling or breathing difficulty requires immediate emergency treatment.
Seek emergency care immediately for: rash with difficulty breathing or throat tightening (anaphylaxis); a non-blanching purpuric rash with fever (possible meningococcal disease); rapidly spreading blistering rash with skin pain and mucous membrane involvement (possible SJS/TEN); or rash with fever, facial swelling, and lymph node enlargement after a new medication (possible DRESS). For any of these, call 911 or go directly to an emergency department — do not wait for a dermatology appointment.

